Lesson 9: Common ENT Problems
Contents
Introduction:
You are welcome to this unit on common Ear, Nose and Throat (ENT) problems. As you may recall in Unit 8, you were told that some of the acute respiratory infections such as acute otitis media would be discussed in unit 9. Remember that there are many diseases of the ENT, but in this unit we shall limit ourselves to the common childhood illnesses such as:
- Blocked nose or nasal discharge
- Ear pain
- Ear discharge
- Tender swelling behind the ear
- Sore throat
- Foreign bodies
By the end of this unit you should be able to:
|
Management of the Child with an Ear Problem
Here you will learn how to assess, classify the illness and give the appropriate treatment of a child with an ear problem. You should remember that the ear is part of the respiratory tract. It is connected to the throat (pharynx) by the Eustachian tube. An acute ear infection is infection of the ear lasting 14 days or less. A chronic ear infection lasts more than 14 days. What are the causes of ear infection? The ears can become infected when there is an infection of the nose or throat. The same microorganisms that cause infection in the nose or throat are also the ones that cause infection of the ear. The bacteria most commonly responsible are Streptococcus pneumoniae and Haemophilus influenzae.
Signs and symptoms of ear problems:
A child with an ear problem has some or all of the following signs and symptoms:
- Pain
- Fever
- Pus discharge from the ears
The dangers of ear infection
Infections of the ear rarely cause death, but they can cause many days of sickness in children. If an ear infection is not identified and treated early, it can put the child in danger of the following:
- Infection of the bone behind the ear called mastoiditis.
- Meningitis or encephalitis (infection of the brain).
- Deafness
- Developmental and learning problems.
Diagnosis
To diagnose an ear infection, you must assess the child correctly. Follow the steps below:
Step One: Assess the Child
Assess the child by asking the mother several questions.
Ask the mother or caretaker
- Does the child have ear pain?
- Ear pain may mean an infection
- Does the child have pus draining from the ear? If so, for how long?
- Pus draining from the ear is a sign of infection even if the child no longer has pain.
|
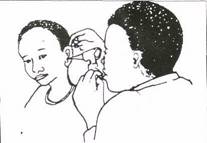
Note that it is important to pull the ear up and back to straighten the external ear canal
|
Look and Feel
- Inspect the pinna for any boils or sores.
- Pull the ear gently in all directions. If this causes pain, then that is a clue that the infection is probably in the outer ear.
- Look for pus draining from the ear or for a red immobile eardrum (you can use an otoscope if you have one).
- Look to see if a foreign object is in the ear.
- Feel for tender swelling behind the ear.
- In young infants, the swelling may be above the ear.
Examine the Ear
To examine the ear, the patient is placed correctly on the mother’s lap. The child is secured firmly by the mother holding the child’s hands with one hand and his head with her other hand. See Fig. 9.1. If you have an assistant, he/she can help you to hold the child’s head. You should sit at the side of the patient with your eyes at the same level as the child’s ears (the organ to be examined). The distance is usually 30cm from the patients head. The hand holding the otoscope is placed on the child’s head. Should the child move the head, the otoscope moves with the head, thus avoiding perforating an inflamed tympanic membrane.
ASSESS ASK • Does the child have ear pain? • Does the child have pus draining from the ear? • If so, for how long? LOOK, FEEL: • Look for pus draining from the ear or for a red, immobile ear drum • Feel for tender swelling behind the ear. STEP TWO: CLASSIFY THE ILLNESS AND TREAT IT: You will have to classify a child with an ear problem as having one of the following: • Acute ear infection (Acute otitis media) • Mastoiditis • Chronic ear infection Let us now discuss how you should manage each of these conditions. 1) Acute ear infection: A child who has pus draining from the ear for less than two weeks, ear pain, or a red immobile ear drum (seen by otoscopy) is classified as having an Acute Ear Infection, commonly known as acute otitis media. If you find a foreign object lodged in the ear, refer the child to a hospital for removal of the object. Management of a child with acute ear infection. Acute ear infection is managed by • Relieving pain with analgesics such as Paracetamol. • Giving the child an antibiotic to treat the acute ear infection. • Drying the ear by mopping if pus is draining from the ear (ear wicking). • Giving the patient a nasal decongestant, such as 3-4 drops of epinephrine since blocked Eustachian tubes often cause otitis media. A decongestant helps in opening the Eustachian tubes if they are blocked at their opening into the throat. • Following-up the patient daily after starting the treatment and referring the patient to the hospital if there is no improvement in the condition. In some rural areas this may be a problem. In that case, the patient is seen as frequently as possible until the signs and symptoms have cleared. • Seeing a patient who is improving again after a few days in order to check for the very serious complications of otitis media.
The child with acute otitis media may have a mild hearing loss that will probably last for some time after healing. If the child is in school child, the teacher should be informed about this temporary hearing loss.
Once the infection has healed, you should ask the patient to come back in about 2-3 months. At this visit, you should do a hearing test. If there is any loss of hearing, you should refer the patient to a doctor.
Mastoiditis: This is an infection of the air cavities in the mastoid bone. Mastoiditis results from the spread of the infection from the middle ear. If the patient feels pain when you press or tap the on the mastoid bone, then you should assume that the infection has spread to the mastoid cavities. Therefore, a child who has tender swelling behind the ear (in infants, the swelling may be above the ear) is classified as having mastoiditis.
Management of a child with mastoiditis in your health facility. A child with mastoiditis needs antibiotic treatment and may require surgery. The child is URGENTLY referred to the hospital after a first dose of antibiotics (see Table 9.1.
Table 9.1: Oral Antibiotics for Ear Infections
TREATMENT OF AN EAR INFECTION WITH ORAL ANTIBIOTICS Give first dose of antibiotic in clinic. Instruct the mother on how to give the antibiotic for seven days at home
Age or Weight COTRIMOXAZOLE Trimethopim + sulphamethoxazole *2 times daily for 7 days 8 mg TMP + 40 mg SMX per kg per day AMOXYCILLIN
- 3 times daily for 7 days 40 mg / kg / day
AMPICILLIN
- 4 times daily for 7 days 75 mg / kg / day
Adult tablet Single strength (80 mg TMP+ 400 mg SMX Paediatric tablet (20 mg. TMP + 100 mg SMX) Syrup (40 mg TMP+ 200 mg SMX per 5ml) Capsules 250 mg Syrup 125 mg in 5ml Tablets 250 mg. Syrup 250 mg in 5ml
<2 mos or <5kg ‘/4# 1# 2.5ml # •/4 2.5ml •/2 2.5 ml
2 to 12 mos (6-9 kg) ‘/2 2 5ml !6 5ml 1 5ml
12 mos to 5 yrs (10-19 kg) 1 3 7.5ml 1 10ml 1 5ml
Adults 2
2
2
If the child is less than 1 month old, give 1/2 paediatric tablet or 1.25 ml syrup twice daily. Avoid cotrimoxazole in premature or jaundiced infants less than 1 month of age.
Child Health Course Unit 9
Alternatively: You can use CEFACLOR in a dose of 30 mg per kg per day
3. Chronic Ear Infection: Classify a child who has pus draining from the ear for more than two weeks as having a Chronic Ear Infection, also called chronic otitis media. You manage a child with a chronic ear infection by:
a. Repeatedly instructing the child, if old enough to understand, the mother, and the teacher to:
• avoid ear picking, either with fingers or with other things,
• prevent water and dirt from contaminating the ear at hair wash and shower with a piece
of clean cotton soaked with Vaseline or oil and inserted into the external ear canal,
• avoid blocking the ear canal to stop the discharge. We do not block a running nose by putting cotton in the nose. Blocking the external ear canal would provoke more discharge.
REMEMBER to follow up all patients with any ear infection. Adequate treatment of the infection can prevent permanent deafness.
b. Instructing the mother on dry mopping: Using cotton-tipped match sticks, absorbent paper-strips or a clean cloth rolled like a pin you instruct the mother or other family member how to mop as much pus as you can be seen. Good light is used and the cotton-tip is not allowed to enter too deeply. Then the mother or other family member is shown how mopping is done and offered a chance for practising. Using sterile, lukewarm saline solution in a 5 cc syringe, gentle syringing is done only at the clinic. The child’s ear is completely dried for the first time in the health facility. Before the mother leaves the clinic, you should check that she has learnt how to mop the ear correctly.
At home, this dry-mopping should be repeated three times daily until the ear is dry.
Regular controls. The patient is seen once a week or every second week until the ear is dry.
Child Health Course Unit 9 The most important and effective treatment for chronic otitis media is to keep the ear dry by mopping. The microorganisms that cause an infection of the ear are often different after two weeks from those that caused acute ear infections. Thus, antibiotics are usually not effective against a chronic infection. The chart below summarizes the management of the child with an ear infection:
Table 9.2: Classifying the Illness
SIGNS Tender swelling behind the ear • Pus draining from the ear LESS than two weeks, or • Red, immobile ear drum (by otoscopy) Pus draining from the ear two weeks or MORE
CLASSIFY AS MASTOIDITIS ACUTE EAR INFECTION CHRONIC EAR INFECTION
TREATMENT
• Refer URGENTLY to hospital • Give first dose of an antibiotic • Treat fever, if present • Give paracetamol for pain
•Give an oral antibiotic •Dry the ear by mopping • Reassess in five days •Treat fever, if present • Give paracetamol for pain • Dry the ear by mopping • Treat fever, if present • Give paracetamol for pain
9.2: MANAGEMENT OF A CHILD WITH A SORE THROAT You will see many children brought for a sore throat. Often this is not a serious problem. The patient may have a viral infection of the upper respiratory tract (a cold), and his/her throat is irritated. If this is the case, you will simply give the patient treatment for the symptoms and the child will soon get better. But sometimes a sore throat can be a warning of a more serious problem. For example: • If the sore throat is caused by a streptococcal infection, then the patient may develop rheumatic fever, and rheumatic heart disease may follow. • Some serious diseases, like diphtheria and peritonsillar abscesses, can cause a sore throat. A sore throat may be a warning of a serious disease
What causes a sore throat? The most common causes of a sore throat are: • Viral infections: Often a sore throat is part of a general upper respiratory tract infection caused by a cold or flu. Colds and flu are both viral infections as we have seen in Unit 8.
• Bacterial infections: streptococcal, pneumococcal or staphylococcal bacteria may cause bacterial infections of the throat.
• Diphtheria: Rarely, diphtheria bacteria may be the cause of a throat infection. Diphtheria is not a very common illness and everyone should be immunized against it. However, there are still occasional patients with diphtheria (see Unit 5 for more information).
Bacterial throat infection
Signs and symptoms of different kinds of sore throats: Fig. 9.2 presents a diagram of the throat. Note the position of the tonsils and pharynx. It is very difficult clinically to tell the difference between a viral and bacterial throat infection. In this section we will give some helpful hints about recognizing bacterial and viral throat infections.
Fig. 9.2:
Bacterial Throat Infection
Viral Throat Infections: A sore throat caused by a viral infection is usually part of a general upper respiratory tract infection. This means you would expect to find some of the other symptoms of a “cold” such as a runny nose, cough, hoarse voice, or earache. Of course, you will not find all these symptoms in every patient with an upper respiratory tract infection. Signs you should look for include:
• The mucous membranes in the throat and tonsils look red and infected. But usually the throat does not look as red as it does in a patient with a bacterial infection.
• The glands in the neck may be swollen and tender. In a viral infection the glands do not get as swollen and tender as they do in a bacterial infection.
• The patient may have a mild fever.
Fig. 9.3: Anatomy of the Throat
Bacterial Throat Infections: Often the sore throat is the only symptom. The patient experiences one or more of the following symptoms of upper respiratory tract infections:
• The sore throat is usually very painful.
• The tonsils are usually very swollen and inflamed.
• You may see pus on the tonsils. The mucus is yellowish/green.
• The glands in the neck are often very swollen and very tender.
• Usually the patient has a fever.
• It may be very uncomfortable to swallow.
• There may be abdominal pain, vomiting or diarrhoea especially with children.
ACTIVITY A mother has brought her 5-year-old son Peter who complains of a sore throat. What would you ask Peter and his mother?
Compare your answers with mine.
For how long has he had the infection? Viral infections usually last 5-7 days. Bacterial infections may last longer.
Does he have ear pain? Has he been coughing? Viral infection can spread up the Eustachian tubes to the middle ear or down the pharynx to the lungs. If Peter has otitis media or a dry cough as well as a sore throat, then he probably has a viral infection.
Does he have a runny nose? This is more common with viral infections, especially if the fluid coming out of the nose is clear.
Is he coughing up mucus? If the answer is yes, then you must find out the colour of the mucus. Clear mucus usually indicates a viral infection. If the mucus is yellow/green in colour, then Peter probably has a bacterial infection (Note that if the child is coughing, you should assess him for pneumonia also as it was discussed in Unit 8. )
Fig. 9.4: Bacterial?? Viral?? How to examine a patient with a sore throat: • Check his general condition: • Does he have a fever? • Is his heartbeat very fast? • Is he very ill? • Does he have any difficult breathing? Check the lymph glands, especially those in the neck and behind the ears. Look very carefully at the mucous membranes in the mouth, at the tonsils and at the throat. • Are they red and inflammed? • Are the tonsils swollen? • Is there any pus on the tonsils, or near them? Children often have quite large tonsils until the age of about 5 years old. Thereafter, the tonsils get smaller. If you see a young child with large tonsils but no inflammation or any other signs of illness, then there is probably nothing wrong with the child’s tonsils. If the neck glands are also swollen, then the child is referred to a doctor. Examine the ears carefully. Often a child may feel pain in the throat without any throat infection. Such throat pain is referred from an infected ear. Examine the chest: Look for signs of pneumonia such as fast breathing and chest indrawing. After you have taken the history and examined the patient, you will be ready to make the diagnosis. It is often impossible to tell the difference between viral and bacterial throat infections. So for management purposes all sore throats in children should be diagnosed as bacterial throat infections. Diagnosing a Sore Throat: ACTIVITY
Remember that there are two reasons why you should try to tell whether a sore throat has been caused by a virus or by bacteria. What are these two reasons?
Now compare your answers with mine. Firstly, you can treat a bacterial infection with antibiotics. Viral illnesses will not respond to antibiotics. Secondly, streptococcal throat infections may cause rheumatic fever. Rheumatic fever can cause damage to the heart valves. This is called rheumatic heart disease. It is important to treat all cases of streptococcal throat infections with penicillin. Once you have made the diagnosis, you need to decide how to manage the patient.
Fig. 9.5: Eat Paw-paw and Drink Fluids
Managing a Patient with Sore Throat:
For any child with sore throat (viral or bacterial):
• Give paracetamol for pain.
• Treat with benzathine penicillin in order to treat the infection and protect against rheumatic fever.
• If the patient is allergic to penicillin, you can use erythromycin or cotrimoxazole.
• In addition, give the child and the mother the following advice:
• The child should gargle and rinse his mouth with mild salty water.
• The child should try to eat mashed pawpaw to keep the tonsils and pharynx clean.
• The child should drink plenty of fluids.
Children are most likely to get rheumatic fever at ages 3-15 years. It is better not to take a chance so always give an antibiotic for a serious throat infection.
Complications of Throat Infections: There are two important complications of throat infections that you should be able to recognize: peritonsillar abscess and epiglottitis.
1) Peritonsillar abscess (Quinsy): Peri means around, so a peritonsillar abscess is an abscess around or near the tonsils. A large swelling forms around the tonsils. The patient usually cannot open the mouth very widely. You may see pus on the very swollen area around the tonsils. Give the patient procaine penicillin and REFER URGENTLY to a doctor. The danger is that the swelling may grow so large that the patient will have difficulty in breathing. See Fig. 9.6.
Fig. 9.6: Peritonsillar Abscess
2) Epiglottitis: Epiglottitis is the infection of the epiglottis, the flap of tissue that covers the larynx when we swallow food. The epiglottis is swollen and can seen at the back of the throat, looking like a small red marble.
Epiglottitis is very dangerous, because the swollen epiglottis can block the airway, and cause the patient extreme difficulty in breathing. It can also cause death.
A patient with epiglottitis looks very ill, has a high fever and may have saliva dripping out at the side of his/her mouth. As the patient breathes, he/she produces a stridor as if he has croup.
If you suspect that the patient has epiglottitis, do not make the situation worse by looking repeatedly at his throat. This might cause more swelling. Give the patient chloramphenical and REFER URGENTLY to hospital.
3) Other Complications of throat infection include:
• Otitis media
• Pneumonia
• Rheumatic fever
9.3: MANAGEMENT OF A CHILD WITH NASAL DISCHARGE OR A BLOCKED NOSE
A runny or blocked nose is a common complaint in any primary health care clinic. It is also the most obvious symptom of an upper respiratory tract infection or allergy. A clear nasal discharge is almost never a serious problem. It can, however, develop into sinusitis, which needs to be taken seriously.
Nasal discharge is also called rhinorrhoea. It occurs when an infected mucous membrane of the nose or the sinuses produce large amounts of mucus. Inflammation of the nose is called rhinitis and can be caused by infection or allergy. So, rhinorrhoea is a symptom of rhinitis. The infection of the sinuses is called sinusitis and needs to be taken seriously. In both rhinitis and sinusitis, the mucus is discharged through the nose. The discharge is usually clear, but can become yellow green if there is bacterial infection.
Allergies can give a patient quite a lot of discomfort, and may need treatment.
ACTIVITY List some of the common causes of rhinitis:
Common causes of rhinitis: The most common causes of rhinitis are: • Viral upper respiratory tract infection - the common cold • Allergies such as hay fever • Bacterial infection: This is sometimes the primary cause of a nasal discharge. Other times, patients develop a bacterial infection after a viral infection. This is called a secondary bacterial infection. A foreign body stuck in the nose may resemble rhinitis by causing a nasal discharge. It is unusual but it does happen sometimes, especially with young children. It is characterized by a nasal discharge of one side only. You now know the most common causes of rhinitis. Next we will describe how these conditions present and how to manage them. Signs, symptoms and management of rhinitis: Remember that rhinitis is an inflammation of the nose and causes nasal discharge. Symptoms of rhinitis include: • Usually low grade fever • A clear nasal discharge with nasal obstruction • Headache and pain in the muscles • Sore or itchy throat with or without hoarse voice • Occasionally signs of otitis media, especially in young children. The symptoms may vary slightly depending on whether the cause is viral or bacterial. Basically, the above are the signs and symptoms of a cold. You will not find all the signs and symptoms in each case. Management: 1) Supportive treatment • Reassure the mother that there is nothing seriously wrong with her child. Tell her that the child will get better in a few days. • Steam inhalations might work. Teach her how to do this. • Give paracetamol to relieve sore throat and headache. • Follow up in a few days to be sure that the patient is improving. • It is only necessary to give antibiotics such as cotrimoxazole if the discharge does not clear up or if the infection spreads to the sinuses. When you are examining a patient with a purulent nasal discharge, you should check to see whether they also have sinusitis. Sinusitis can develop serious consequences, and should be treated with antibiotics. 9.4 MANAGEMENT OF A CHILD WITH SINUSITIS Definition of sinusitis. What is sinusitis? Sinuses are empty spaces in the skull. They are found behind the nose, behind the cheeks, and above the eyes. The sinuses are lined with mucous membranes. Normally the sinuses produce a small amount of mucus that drains into the nose. A bacterial infection of the upper respiratory tract can spread to the sinuses. When this happens, the mucous membranes in the sinuses become inflammed and produce large amounts of mucus. We call this sinusitis. The outlet of the sinus may become blocked. This causes a build-up of mucus and pus in the sinus. Symptoms of sinusitis include: • a recent cold or allergic rhinitis • a purulent nasal discharge, and often nasal blockage. • a feeling of fullness in the cheeks and head, especially when leaning forward. • a headache • a cough Signs of sinusitis include: • fever. • tenderness on palpation over the sinuses and on pressing gently on the eyes and above the eye,. • red and inflammed mucous membranes of the nose. • a yellow-green (purulent) discharge in the nose or a postnasal drip.
Management of Sinusitis: The aims of treating sinusitis are: • Clearing any blockage so that the sinuses will drain. • Treating the infection,
These aims are achieved through:
S+aen inhalation Fig. 9.9: Steam Inhalation Regular steam inhalation which helps to clear the blocked sinuses and to drain the mucus. Giving decongestants to improve the drainage of mucus. Giving antibiotics, such as cotrimoxazole to treat the infection Following up the patient in two days. Referring the patient to a doctor if the sinusitis does not clear up, where balloon sinuplasty might be recommended
Complications of sinusitis: If sinusitis does not clear up, it can lead to some dangerous complications. These complications result from the spread of the infection to the neighbouring tissues and include:
• Orbital cellulitis (infection of the orbit),
• Periorbital cellulitis (infection of the tissues surrounding the eye).
• Osteomyelitis (infection of the bone surrounding the sinuses)
• brain abscess or meningitis.
Some of these complications may require surgery. A complication must be suspected if a patient with sinusitis develops any of these symptoms:
• Severe headaches
• A stiff neck
• Severe swelling in the face
• Swelling of the eyelids
• Restricted movement of an eye
Give the patient an injection of benzyl penicillin, and REFER him to a doctor immediately.
(9.5. MANAGING A CHILD WITH ALLERGIC RHINITIS OR HAY FEVER:
Definition of allergic rhinitis or hay fever.
Allergic rhinitis or hay fever is inflammation of the mucous membrane of the nose caused by an abnormal reaction to contact with certain substances called allergenes. Often the allergic reaction causes abrupt sneezing, running nose, and watering of the eyes.
Causes of allergic rhinitis include:
• Flowers, grass and pollen especially from flowers.
• Hair from dogs and cats.
• House dust mites contained in the house dust.
• Some foods - especially fruit drinks.
• Moulds (tiny fungi)
The symptoms and signs of allergic rhinitis are:
• repeated attacks of hay fever (sneezing, clear rhinorrhoea, nasal itching and nasal congestion and excessive tearing) The patient may be able to tell you what particular thing is causing him/her to sneeze.
• asthma or eczema.
• Conjuctival oedema, itching, tearing and redness.
• Clear watery nasal discharge associated with sneezing, itching and nasal congestion.
• Absence of signs of inflammation in other parts of the upper respiratory tract.
ACTIVITY
How do you manage a patient with severe rhinitis?
When patients suffer from chronic allergies and the accompanying rhinitis, there are a number of things you can suggest that can make them more comfortable. Above all, be supportive and explain what the condition is all about.
• Advise patients to avoid the thing that causes the hay fever. Of course, if it is pollen and grass this is not very easy. But dogs and cats should not be allowed in the home. If dust is the problem, then the patient should wash curtains, carpets and bedspreads often to clean the dust out. Encasing the mattress, pillow and covers in mackintosh or rexine is the most effective way of reducing the house dust mite allergen. The patient should avoid cold drinks with preservatives.
• Regular steam inhalations help.
• Preparations like chloropheniramine (piriton) have antihistaminic and decongestant effects. These preparations reduce sneezing and rhinorrhoea in mild intermittent allergic rhinitis. Pseudoephedrine, a vasoconstrictor may be used to treat nasal congestion if it is given for less than 5 days, once a month. Patients with severe persistent symptoms are referred to the doctor.
Fig. 9.10: Be Supportive to Your Patients
Very bad hay fever can make life very uncomfortable for a patient. Bad, chronic cases of allergic rhinitis should be referred to a doctor. The doctor may do tests, but quite often they are unnecessary. Medicine for allergic rhinitis is quite expensive and it is best if prescribed by a specialist.
You have learned that viral and bacterial rhinitis, sinusitis and allergies can all cause nasal discharge. Foreign bodies stuck in the nose can also cause a nasal discharge. You have learned how to manage these problems and how to help your patients cope with nasal discharge.
We have come to the end of Unit 9. We hope you have found it interesting and practical, and that it will help to improve your clinical skills.
Take a rest, and then complete the Tutor Marked Assignment. Send it to us and we will mark it and send it back to you with our comments.
MOH/AMREF DISTANCE EDUCATION COURSE
Number Name . Address.
Child Health Course
Unit 9: Assignment Common Ear, Nose and Throat Problems
Answer all the questions, before sending the assignment. If you have any problem with any of the question look back on the lesson. If you still having a problem, write for more clarification.
1. Lucia who has been brought to your clinic is 7 years old with a hearing impairment. Whenever she goes to swim or puts her head in water, her ears get discharge. She has been seen in our clinic where they cleaned her ears and put in some drops. On examination, you find she has pus in both ears.
a) What do you think is the problem with Lucia?
b) How will you manage her case?
2. Bosco is 4 years old. His ear has been running for quite some time and he complains of pain and buzzing in the right ear. He has no upper respiratory problems and he seldom has a running nose
a. What else would you ask the mother?
b. What would you examine the child? c. What do you think is the problem with Bosco? d. How would you manage the case?
3. Salome is 6 years old and has had a discharging ear for some time. For the last 3 days has had a severe headache, fever and is rather sleepy. a. What else would you ask Salome? b. How would you examine her?
c. What do you think is her problem?
d. How would you manage the case?
4. A 5 year old is brought to your clinic by his older sister. The child has a nose bleed, and his shirt is covered with blood.
a) What measures would you take to stop the bleeding?
b) If that does not work what would you do next?
5. A mother brings her 30 month old child to your clinic because she has had a sore throat and fever for 3 days. The child has refused to eat and has vomited a few times. When you examine her, you find she has a fever of 40 C. Her eyes are clear, her ear drums look normal, the throat is very red and the tonsils are swollen with pus on their surface. The neck is not stiff, but there are big tender lymph glands near the angles of the jaw. The mother tells you that this is the third time this year that the child has had this problem.
a) What do you think is wrong with the child?
b)How would you manage this child?
Congratulations! You have now come to the end of this unit, remember to indicate your Personal File Number, names and address before sending it.