Lesson 2: Maternal Nutrition during Pregnancy and Lactation
Contents
Introduction
Nutrition and infection and disease interact in a complex. The nutritional status of an individual will affect the incidence, severity and duration of infection.
Infection can induce malnutrition by interrupting food intake through anorexia or modifying nutritional requirements. Nutrition can modify the complex array of host responses aimed at eliminating infectious organisms.
Some diseases are nutritionally related either through excess or deficiency of certain nutrients. This unit will provide you with the basic knowledge that you need to understand how nutrition, infection and disease relate to each other. The unit also describes what can be done in order to break the Nutrition – infection cycle.
By the end of this unit, you should be able to:
|
Definition of Terms
Nutrition is a process by which food is eaten, digested and utilized in the body for production of energy, growth, maintenance and regulation of body functions.
Infection is the invasion of the body by organisms that cause disease.
Disease is the interruption, cessation or disorder of body functions, systems or organs. It is usually characterized by a recognized etiologic agent, identifiable signs and symptoms with consistent anatomical alterations.
Health is a state of physical, mental and social well being. |
Lesson
The Relationship Between Nutrition and Infection
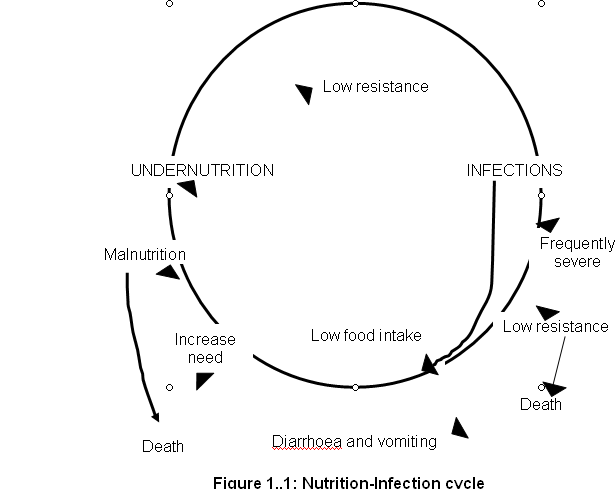
There is a very important relationship between nutrition and infection, which particularly affects children as illustrated in Figure 1.1. Poor nutrition lowers the resistance of the whole body to infections.
Undernourished children are more prone to infection, recover from illness more slowly and frequently die from infections. Malnutrition tends to be under-reported in disease and mortality statistics because a sick child with malnutrition is likely to develop complications such as gastroenteritis, which lead to death. The deaths are then reported as being due to these diseases rather than malnutrition. But under nutrition and malnutrition are by themselves serious problems, even when they are the mild or moderate form, as they influence the onset and outcome of infections. A malnourished child is more likely to get infections more often and more seriously than a well-nourished child.
To treat a malnourished child, it is important to treat any infection that the child may have. However, it is better to prevent the malnutrition by immunizing against the infections.
Infections cause fever, loss of appetite, diarrhoea and vomiting, all of which interfere with the intake and absorption of food, and malnutrition follows. Fever and the repair of damaged cells also increase the need for food. Therefore, with less intake and greater need for food, the infected child with poor reserves is easily tipped into a state of malnutrition.
Loss of appetite, known as anorexia, is another factor in the relationship between infection and nutrition. When a child is ill with an infectious disease he often has a poor appetite and therefore reduced food intake.
Infections and parasites may be important not only in the aetiology of Protein-Energy-Malnutrition and anaemia but may also aggravate condition such as xerophthalmia (corneal ulceration) as a result of Vitamin A deficiency, an important cause of blindness. We shall discuss Vitamin A in detail in Unit 5 when we are discussing micronutrients.
Because most infections lead to undernutrition, and under-nutrition, in turn, makes a child more susceptible to infections, a cycle of infection / undernutrition frequently develops with disastrous results. This is illustrated in Figure 1.1.
It is quite clear that infections make malnutrition worse, and poor nutrition increases the severity of infectious diseases.
Let us now discuss the relationship between nutrition and disease.
The Relationship Between Nutrition and Disease
Do Activity 1/1 below. The activity should take you 5 minutes to complete.
| ACTIVITY 1/1
Explain how nutrition and disease relate to each other. ………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………….
…………………………………………………………………………………
|
Different diseases and infections affect the nutrition of a child. We have known for some time that infectious childhood diseases like measles and whooping cough lead to malnutrition. A child with measles may have sores in his or her mouth, which will prevent him or her from eating food, because it hurts. The child may also not have appetite and ends up getting malnutrition. Whooping cough makes the child to vomit as the child coughs. If a child vomits he or she is losing fluids and nutrients. This interferes with food intake and the child gets malnutrition. Even healthy children who get measles lose weight; because in many African traditions, children with measles are not allowed to eat certain types of foods mainly meat, milk, fish and eggs. They then end up getting a severe form of malnutrition. If a child has fever, his or her body uses more energy. Because little food is taken in the child’s body will use its own tissues for energy. This makes the child grow weak and malnourished.
Of all the infectious diseases, diarrhoea is the most important cause of malnutrition. Dirrhoea is common during the weaning period, and it is termed “weanling diarrhoea”.
Several different things can cause diarrhoea. For example, children can get diarroea when they play in dirty places and when they eat unclean food, or are bottle-fed with dirty bottles. Children also get diahhorea if their mothers had dirty hands while they prepared food.
Figure 1.2: This child may get diarrhoea as she is being fed from a dirty bottle.
It is possible that Protein-Energy Malnutrition can be precipitated by an attack of diarrhoea, because diarrhoea seriously interferes with the absorption of food from the gastrointestinal tract in a child who is already poorly nourished. Diarrhoea in an African toddler is frequently treated at home with a bland, mainly carbohydrate diet or by semi-starvation, thus further reducing the food intake.
In many communities it is a common practice to starve children when they have diarrhoea. This is wrong because it causes malnutrition, which will make the child have diarrhoea more frequently.
Antibiotics given for diarrhoea at the health centre or hospital Outpatient Department may interfere with the normal intestinal flora and in this way, they worsen the nutritional state of the child. The old injunction to “starve a fever” is of doubtful validity, and this practice may have serious consequences for the child who is already undernourished. Non-infective diarrhoea may follow a change of diet, this occurs when a child is suddenly taken off the breast and is expected to share the often unsuitable family diet. A child fed on breast milk receives a diet with a high nutritive value and which is less likely to be contaminated than other foods. The child taken off the breast onto a starchy diet may develop a lowered resistance and is more exposed to gastrointestinal infections.
While diarrhoea can cause malnutrition, kwashiorkor and marasmus are very frequently accompanied by diarrhoea. A grossly deficient diet, especially one deficient in protein, may lead to a reduced secretion of digestive enzymes, particularly form the pancreas. This lack of enzymes may cause non-infective metabolic diarrhoea. Protein-energy malnutrition may therefore be caused by, as well as be a cause of, diarrhoea.
This relationship between diarrhoea and Protein-Energy Malnutrition is stressed because it is desirable that public health workers consider improving nutrition as a means of lessening the impact of diarrhoeal diseases, and also that medical nutritionists consider using public-health measures to reduce the prevalence of malnutrition.
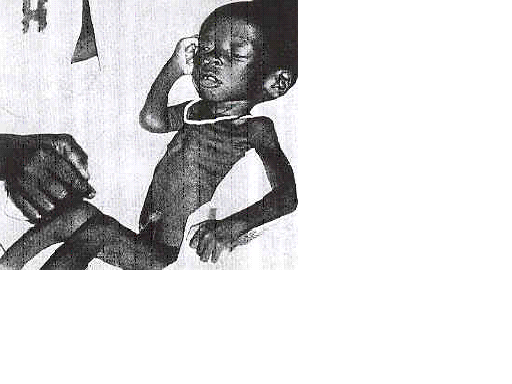
Tuberculosis is another important disease nutritionally. In infancy this disease is often associated with nutritional marasmus (see Fig. 1.3) The patient with pulmonary tuberculosis nearly always shows signs of malnutrition.
Malaria, another great public health problem, tends to be aggravated by malnutrition. Malaria is normally accompanied by high fever and this can increase calorie demand.
Intestinal parasites, which may be extremely common, are also closely linked with malnutrition. It is well established that hookworms, which suck blood, cause a loss of iron and other nutrients.
Figure 1.3: Child with marasmus and tuberculosis
But how can we break the nutrition-infection cycle? It is important that you learn how to break the nutrition-infection cycle.
This knowledge will help you to guide the community in preventing diseases.
Let us now discuss how to break the nutrition-infection cycle.
Interrupting the Nutrition-Infection Cycle
Stop for a while and do Activity 1/2 below. Spend not more than 5 minutes on it.
ACTIVITY 1/2
What can you do in a community to break the Nutrition-infection cycle? ………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
……………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
|
To break the Nutrition-infection cycle, the following can be done:
- Educate the community on the importance of immunizing children against the childhood immunisable diseases like measles, tuberculosis and whooping cough.
- Sensitize the community on the importance of having even distribution of food in a family.
- Detect and treat early illnesses in adults and children.
- Sensitize the community on better farming methods, like clearing the land at the right time, and using irrigation and fertilizer, if necessary. Also harvesting at the right time and having safe storage of food. This can reduce shortage of food in the community.
- Advise the community to use adequate and safe water.
People should make efforts to have both large quantity and better quality of water. If there is no piped water, they can be advised to collect water from protected sources.
Drinking water should be taken from the cleanest possible source. Unless you are sure that the water is safe, it should be boiled before drinking.
- Advise the community to have and use latrines properly.
- Create awareness about good nutrition and child health in schools, families and communities.
- Advice on observance of good hygiene measures
Another way of breaking the nutrition – infection cycle is management of infectious diseases.
It is important that individuals with infectious diseases are given both specific treatment and general treatment. Specific treatment is giving special medicines that kill particular infecting germs or parasites. Tuberculosis and malaria are examples of diseases that require specific treatment. Tuberculosis treatment must continue for a full year, while malaria treatment may start to be effective within a few hours. Both diseases also need general treatment. General treatment includes: a nutritious diet; fresh air and rest.
Measles is a disease for which there is no specific treatment. The most important part of the general treatment is a nutritious diet.
How easy is it to feed a child with measles? Have you ever had the experience of feeding a child with measles?
It may not be easy to feed the child at first, because the child may have a sore mouth and no appetite. When you put food in the mouth when there are sores it hurts. The parents and caretakers of such children will also need to be gently persuaded to help feed the m. Soft foods of the type that the child likes most should be tried first. As a rule, little nutritious food should be given often. The child should be given a mixed diet rich in protein supplements. Mothers should be encouraged to breastfeed their babies. Correct feeding is the best way to help the child recover from the disease.
The treatment of any infection is not complete until the patient begins to eat normally. The best measure of nutrition for a child during and after illness is the weight of the child. Nutritional improvement is shown in two ways:
- The child’s weight should be more than it was before illness;
- The growth curve on the chart should be going upwards.
It is therefore important to have the child weighed and checked regularly to keep a good chart.
Until there are signs of nutritional recovery, the child should receive extra food. This food can be an extra meal each day or an extra helping at each meal. This is an essential part of the treatment. Proper feeding is as important as giving any medicine, and it is more important than giving any health tonic.
Prevention of Infectious Diseases
Before you continue reading, do Activity 1/3 below. It should take you 5 minutes to complete it.
ACTIVITY 1/3
What measures would you take to prevent infectious diseases in your Community? ………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
………………………………………………………………………………..
……….………………………………………………………………………..
………………………………………………………………………………..
|
Most common serious infectious diseases can be prevented. This can be done in two ways which include:
- Decreasing the chances of individuals or the community, coming into contact with the germs or parasites through improving the environment.
- Improving the defense mechanism of individuals so that, if they are infected, the disease does not become severe. This can be done through immunization.
Let us discuss each of the above points in detail.
Improving the Environment
The first method of preventing infectious diseases is improving the environment, or the area in which people live.
The availability of water for drinking, cooking, and washing is one of the main reasons why rural communities develop in a particular area. However, most sources of water in the community, especially in rural areas, are unprotected and easily polluted.
Man is the reservoir host for many disease causing organisms. For example, the unsatisfactory disposal of excreta leads to an increase in faecal–oral transmission and spread of diseases like diarrhoea which interfer with one’s nutrition.
Inadequate housing which leads to over crowding, lack of ventilation, and dampness favours the transmission of airborne diseases. Poor siting of houses for example, too close to where animals are kept, encourages flies.
Poor disposal of rubbish encourages both flies, and rats. This also increases the transmission of vector-borne diseases, for example plague.
The control of the factors in the physical environment that may cause disease is often called “Environmental Sanitation”.
It is the responsibility of all health workers to help the community improve the environment. You can do this by giving health education to the community, and setting an example in your own home, or at your health facility. You can also do it by assisting various community development projects in your service area. It is essential that you have a little background knowledge to enable you to do the simple things required in villages yourself. You don’t need to be an Environmental Health Officer to do this.
Control of the Environment is the responsibility of all health workers.
Let us now discuss the factors which cause diseases in our environment and how to control them.
(i) Water
Water can affect health in a number of different ways. Lack of adequate and safe water for personal hygiene may result in the increased transmission of some diseases called water-washed diseases, such as diarrhoea and dysentery. Water may also carry the organisms of specific diseases called water-borne diseases, such as typhoid, cholera, poliomyelitis, and hepatitis A.
Some diseases like diarrhoea, typhoid and cholera interfere with individual’s nutrition due to loss of nutrients. Children are the most affected.
As a health worker, therefore, you should encourage people to use adequate and safe water. They should collect water from protected water sources, for example protected springs, taps and bore holes. You should advise them to wash hands after using toilet, before handling food and before feeding children. This will help to prevent water – washed and water borne diseases.
Drinking water should be taken from the cleanest possible source. Unless you are sure that the water is safe, it should be boiled before drinking. Water should be kept in clean, covered containers and used only for drinking. See Figure 1.5.
Figure 1.5: Keeping drinking water clean
(ii) Human waste disposal
- The hygienic disposal of human waste is important because the infective organisms for many diseases leave the body in faeces and some in the urine. The following diseases can all be spread from faeces. - Typhoid fevers; - Cholera; - Poliomyelitis; - Infective hepatitis A; - Intestinal worms.
If a person defaecates near the source of water, the stool goes into the water, and later someone drinks water from the same source.
Figure 1.6: A child defaecating near the source of water.
Or the germs may get onto a person’s hands if the person does not wash his or her hands after passing stools. This person can infect food if he or she does not wash hands before preparing or eating food. The food may cause diarrhoea in people who eat it.
It is therefore, important to dispose of excreta safely because excreta can be the source of so much sickness in the community if it is accessible to flies and fingers which transfer to food. This is the Four-F connection. See Figure 1.7
Figure 1.7: The Four-F connection
The Four-F connection is often called the faecal-oral route of transmission. Many people in rural areas still defaecate in the bush. To improve sanitation it is necessary to help people understand the importance of using pit latrines. They should keep pit latrines clean. Stools passed by children near the house should be take away and put in a latrine or buried. There are many local customs and taboos that make this difficult. You must find out what these are in order to be able to change them gradually.
(iii) Food hygiene
Food as well as being essential for growth, development, and energy, may also be responsible for the spread of a number of important diseases. The aims of food hygiene is to prevent food going bad or becoming contaminated at any stage. At the stage of production, collection, storage, preparation or consumption.
Contamination occurs most commonly from excreta on people’s fingers, or flies, as I described in the previous section. Food may also be contaminated with the infections of the skin, especially the hands of food handlers.
Figure 1.9: This child is playing in a dirty place and eating
dirty food. He is likely to get diarrhoea.
Figure 1.10: The mother of this child has not washed her hands before feeding her child and is feeding her in dirty surroundings. The child may get diarrhoea. Health education is extremely important for all who handle food, at any stage from production to eating.
As fresh food is not always available, various methods of preserving and storing food have been developed.
If bacteria can be prevented from getting into food, or conditions unfavourable to their development can be created, then food will remain good for a longer time.
The main methods of food preservation include:
• Drying or smoking. • Saturation of food with salt. • Proper use of refrigeration.
You should teach your community how to preserve food to avoid eating contaminated food that can cause infection.
(iv) Refuse
Refuse, or solid waste, is produced by man all the time wherever he lives, works or happens to be.
The indiscriminate disposal of refuse is unsightly and produces offensive smell. It attracts insects and vermin – particularly flies, cockroaches and rats, and may be involved in the spread of diseases.
Refuse should be put in a pit or burnt so as to keep the area around the houses clean and to avoid spread of diseases like diarrhoea which may lead to malnutrition.
(v) Control of vectors
Mosquitoes
Malaria which is a common killer disease in Kenya is transmitted by mosquitoes. Mosquitoes depend upon water for breeding. An important way of controlling mosquitoes, therefore is by removing all water breeding sites. The nuisance and danger from mosquitoes can be reduced if every community member does his part to fight them in the following ways:
• Reducing their numbers by: - Draining or filling in water holes and ditches in or near houses. - Clearing bushes and grass along the banks of rivers and ponds and in the village. Mosquitoes breed in wet places and long grass prevents drying; cutting the grass will also let the river water flow fast and wash the larvae away. - Collecting and disposing of all containers likely to hold water. This includes tins, broken pieces of water pots, old motor car tyres, broken pieces of cups and glasses, etc.
• Preventing mosquitoes from biting:
- Using bed nets, preferably treated with Permethrin. This insecticide can also be applied to curtains and wall clothes. - Bedrooms and sitting rooms should have windows screened with mosquito-proof wire gauze. - Using mosquito-repellent coils and residual insecticide sprays. These help but are expensive.
Rodents
Rats and mice live and multiply rapidly where there is a low standard of sanitation and where human food is easily accessible. Rats enter people’s houses to find food. It may be waste food, remains of food on unwashed utensils or any food which is not kept closed up in rat-proof containers. You should teach every member of the community should do the following to control this nuisance and health hazard: - Arrange proper storage, collection and disposal of all types of rubbish. - Remove bush and long grass in and around the home. - Seal rodent holes with earth or other suitable rat-proof material. - Store food and food leftovers in properly closed containers. - Uncooked food like rice, maize, millet, cassava, beans, etc., should be stored in rat-proof stores outside the main building. This can be in form of a store or a granary. - When there is a big population of rodents, people may need to hunt them with sticks. - Break-back or cage traps can be used. - Pets such as cats and dogs also help to control rats and mice.
Houseflies
Flies breed and feed on decaying matter such as vegetable refuse, animal carcasses and particularly, on feaces. They transfer bacteria from the decaying matter onto human food, skin and eyes when they land on them. Flies around people are looking for food. This food may be food scraps, discharges from eyes or sores, food around the mouths of children, or faeces. Reducing food for flies will in turn reduce flies near people. As with rat, the less you feed them the less they come to you.
You should sensitize the community about fly habits so they will understand when asked to help control them. They can control them by:
- Disposing of all refuse, any decaying matter, carcasses and faecal matter properly – that is by burying, burning or composting for fertilizer.
- Keeping all house surroundings clean all the time.
- Keeping the houses themselves clean, that is placing all leftover food in covered dustbins.
- Keeping clean all food vessels and utensils.
- Protecting food from flies. The use of food and meat safes are recommended for this purpose.
To stop children and adults getting diseases like dysentery, diarrhoea, typhoid, cholera and hepatitis A, you should advice people in your community to:
- Wash their hands before preparing food.
- Wash their hands before eating food.
- Use latrines.
- Quickly clean up the stools of young children and put them in a latrine.
- Keep their houses clean.
- Keep drinking water clean in covered pots.
- Encourage mothers to breast-feed their babies.
- Keep flies and cockroaches away from food by covering it.
People in the community can do the following things to stop children and adults getting diarrhoea (See Figure 1.11 (a), (b), (c), (d) and (e)..
1.5.2 Immunization
The defences of an individual against infections can be improved in a general way or in specific ways. A better state of nutrition means that a child’s defences can function fully against any infections. This is a general improvement. An improvement of the defences against specific infections can be achieved by immunization. A child who has measles once becomes protected against the disease by a special substance that his body makes. This is called “natural immunization”. It is also possible to produce “artificial immunization”. This is done by injecting “weakened” germs into the body. These germs attack the body but are not strong enough to produce the signs of the disease. However, they do cause the body to produce the special substance that kills the disease germs and thus protects the body from future attacks. A substance which can give specific artificial immunization is called a “vaccine”.
There are a number of vaccines which can give immunity against diseases. These are very valuable in protecting the child against dangerous diseases of young children. The vaccines are made and given in different ways and have to be given at about the right age for the best effect. They also need to be given at certain time intervals.
There are eight important and common childhood immunizable diseases for which there are vaccines. These diseases are:
- Measles,
- Tuberculosis,
- Whooping-cough (pertussus),
- Diphtheria,
- Tetanus,
- Poliomyelitis (infantile paralysis),
- Hepatitis B and
- Haemophilus Influenza type b.
The vaccines are given in a particular order, at specific ages and with appropriate intervals of time. The vaccine schedule may differ slightly from one country to another.
Immunization is discussed in detail in the immunization course. If you want to know more about immunization, you are advised to take Distance Learning course on Immunization. You can also visit any library where you can find a variety of books on immunization.
The childhood immunizable diseases often affect the nutrition of a child. A child with Whooping cough, for example, vomits after every boot of cough. Each time the child vomits he or she is losing fluids and nourishment.
A child with measles has a cough, a fever and sore mouth. He or she may not want to eat. With fever, his or her body uses more energy. Because little food is taken in, the child’s body will use its own tissues for energy. This makes the child grow thin, weak and malnourished.
Sometime parents do not feed a child who is ill. They think that because the child is not vomiting or has diarrhoea, he or she should not eat. This is very dangerous. Children who are not fed when they have diarrhoea, measles or other infections will begin to lose weight. They will become malnourished. A malnourished child will get infections more easily. A sick child, therefore, needs food.
You should, therefore, advise the community to take their children to a health facility where they will be given immunizations. An immunisation helps the child’s body to fight the germs that cause some infections and diseases. Immunisations are often given in the form of an injection.
Besides improving on environmental sanitation and immunizing children, a child should be given enough of the right kinds of foods to be strong and healthy. The human body has ways of fighting germs and infection. If a child is healthy, strong and well fed, his or her body can fight germs better than if the child is weak and malnourished.
You can find out useful information about infections in the community. The information will help you, as a health worker, to decide what plans to make to help protect children from infections.
Do Activity 2/2. Let your in-charge and your colleagues give you a feedback.
| ACTIVITY 2/2
Visit any community in your service area and collect data on infectious
Diseases using the questions below.
Analyse your data and present your findings to your health facility
in-charge and your colleagues.
Together with your in-charge and your colleagues, plan how you can
help the community to prevent the diseases you will have identified.
|
| QUESTIONS:
1. Which infectious diseases occur in the community, and what are their local names? ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… 2. At what time (season) of the year are these diseases common? ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ………………………………………………………………………………
……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ………………………………………………………………………………
6. Are there special foods or ways of feeding that are used for children with the diseases you listed in Number 1? ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… ……………………………………………………………………………… |
Before we conclude our discussion, let us have the summary of what we have discussed.
| In summary, we have said that poor nutrition lowers the resistance of the whole body to infection. Undernourished children are more prone to infection, recover from illness more slowly and frequently die from infections. Infections make malnutrition worse, and poor nutrition increases the severity of infectious diseases. |
We also said that infectious diseases like measles and whooping cough lead to malnutrition. The treatment of any infection or any infectious disease is not complete until the patient begins to eat normally.
Finally, we said that three main ways of preventing infectious diseases are by improving the environment, immunizing children and by having proper nutrition.
Congratulations!
You have come to the end of this Unit. I hope you learnt a lot from this Unit. Review your answers to the in-built Activities. Look at the objectives of this unit once again. If there is any you are not sure of, review the relevant sections. If you have mastered the content in the unit, put the Study Guide away, take a break then do the Tutor Marked Assignment.
REFERENCE
1. Community Nutrition for Eastern Africa by Ann Burgess. Africa Medical and Research Foundation 1994.
2. Community Health manual for health workers by AMREF.
3. Human Nutrition in Tropical Africa by M.C Latham, Cornell University Ithaca, New York, USA 1981.
4. WHO Geneva 1986: Guidelines for training Community Health workers in nutrition.
5. WHO and UNICEF, Geneva 1989: Nutrition Learning Packages.