Lesson 19: Disability and Rehabilitation Part 1
Contents
- 1 INTRODUCTION:
- 2 19.10: SUMMARY
- 3 PRACTICAL
- 4 Assignment
INTRODUCTION:
In Unit 17 we learnt that children with disabilities tend to become victims of child abuse and neglect. It is often difficult to know how many disabled children we have in our communities because the parents may not always come for help in our health care facilities. As you are well aware, in our communities there are people who believe that disability is a problem that results from a curse, from ancestral spirits or witchcraft. Such people feel that persons with disabilities (PWDs) are a waste of time, a stigma to the family and community, and that they should be kept out of sight. These negative attitudes are caused by ignorance. All health care providers are charged with the responsibility of creating awareness and establishing medical services for PWDs that span the country. You and I can make a difference by promoting equalisation of opportunities for PWDs. One way you can do this is by learning more about disabilities in the following text.
There are several types of disabilities that affect the child. Some have been covered in the preceding units. In units 19 and 20 we shall be looking at movement or physical disabilities.
|
By the end of this unit you will have learnt the following:
|
19.1 WHAT IS DISABILITY
In the management of people with disabilities, we need a clear definition of who is disabled. The definition varies among the health, educational and social service workers.
What is disability in the health context?
According to the World Health Organisation’s definition, disability is any restriction or lack of ability (resulting from impairment) to perform an activity in the manner or within the range considered normal for a human being.
Disability refers to the person’s actions, such as the inability to walk, strange or abnormal behaviour, seeing or hearing difficulties, and so forth.
Let us begin by doing an activity:
|
List five of the most common disabilities you see in your community: _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Now confirm your answers as you read the following discussion.
19.2: TYPES OF DISABILITIES
The five main types of disabilities are:
- Movement or physical disabilities
- Seeing difficulties (blind or low vision)
- Mental disorders (strange behaviour, mental retardation, epilepsy) and mental illness
- Hearing and communication difficulties (deaf or dumb)
- Sensory impairment, such as leprosy
Let us look at each in turn.
19.3: MOVEMENT OR PHYSICAL DISABILITIES
Physical disabilities develop as a result of damage to either nerves, muscle, or bone tissues. These include, for example, amputations, complicated fractures, congenital abnormalities, diseases such as poliomyelitis, or a combination of some or all of the above. In normal circumstances, nerve impulses facilitate muscle contraction, and control muscle function.
Damage to nerves leads to paralysis of muscles, that is, muscles lose the ability to contract, initiate and control motor function. For example, poor obstetrics practice may cause trauma such as brain damage to the newborn at birth, resulting in cerebral palsy, one of the major causes of physical disability.
Congenital abnormalities are deformities that a child is born with, for example a club foot, spina bifida, hydrocephalus, bone and joint malformation. We shall give a brief description of some of the conditions and diseases mentioned that cause physical disability. Let us start with spina bifida and hydrocephalus.
- Spina bifida or Myelomeningocoele:
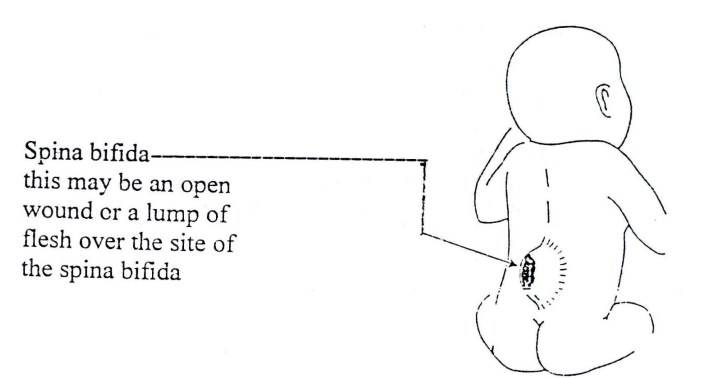
“Spina bifida” comes from two words: “Spina” meaning spine, and “bifida” meaning split or divided. Spina bifida is a defect involving one of the bones of the vertebral column. It occurs in the early stages of development of an unborn child. During the intrauterine development period, some of the bones of the backbone or vertebrae do not close over the centre, leaving the spinal cord or bundle of nerves unprotected. See Fig. 19.1
How does spina bifida occur?
Available literature states that spina bifida is a defect that occurs in the development of the infant’s spine. It occurs within the first 21 days of pregnancy.
The bones of the infant’s spine do not close over the spinal cord as stated above. Part of the spinal cord, which is located under these bones, may be abnormally formed or damaged. A soft, unprotected area will be present on the infant’s back. . Sometimes it is only the meninges that bulge out of the defect (meningocoele) or meninges and nerves (myelomeningocoele). The defect may be covered by skin, or more commonly an open wound that may bulge through the skin. (Fig. 19.1). This bulge is covered by a very thin layer of membrane that may leak liquid from the spinal cord and brain.
Figure 19.1: Spina Bifida
What can be done to prevent spina bifida? There is no single cause for spina bifida. Several factors that, when combined, may lead to spina bifida. One of the factors is folic acid deficiency around the time of conception. Taking folic acid is very important before and during pregnancy. It is very important to realise that neither of the parents is to blame when a baby is born with spina bifida.
The risk of having a baby with spina bifida can be reduced in the following ways:
- Eating a healthy diet before and during pregnancy: eating foods that contain folic acid and Vitamin B12 such as liver and dark green leafy vegetables or by taking folic acid tablets.
- If a woman is taking medicine to control other illnesses such as epilepsy, she may need to take larger amounts of folic acid.
- Not drinking alcohol if pregnancy is being planned.
Yes indeed, there are different types of spina bifida. See Figs. 19.2 a & b
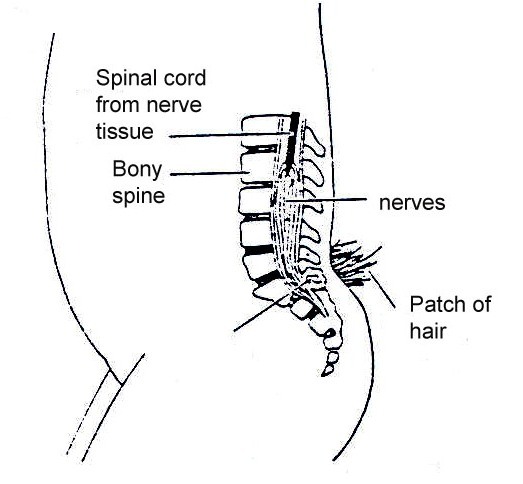
Spina bifida occulta. Occulta is the mildest and most common form in which one or more vertebrae are malformed. The name “occulta,” which means “hidden,” indicates that the malformation, or opening in the spine, is covered by a layer of skin. This form of spina bifida does not usually cause disability unless there is tethering of nerves.
Fig. 19.2a: Spina bifida occulta
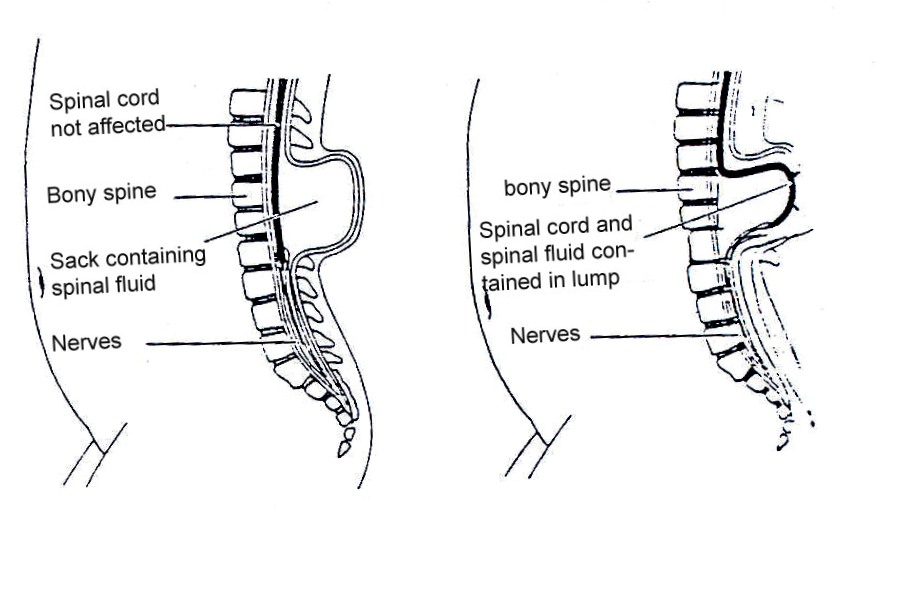
Figure 19.b: Meningocoele and myelomeningocoele
In meningocele, there is only fluid in the sac. This too rarely causes disability
Meningomyelocoele is the most severe and occurs when the spinal cord is exposed through the opening in the spine. This time the nerves are involved and the defect is usually not covered with skin This condition may result in partial or complete paralysis of the parts of the body below the spinal opening. The paralysis may be so severe that the affected individual is unable to walk and may have urinary and bowel dysfunction.
In all these cases the defect may be associated with hydrocephalus (an abnormally high amount of cerebral spinal fluid
How does spina bifida affect the child?
The spinal cord normally carries messages between the brain, and the body and the limbs. These messages help to control movement of the limbs. They also tell the brain about the feelings of touch, pain, and signals from a full bladder or bowel.
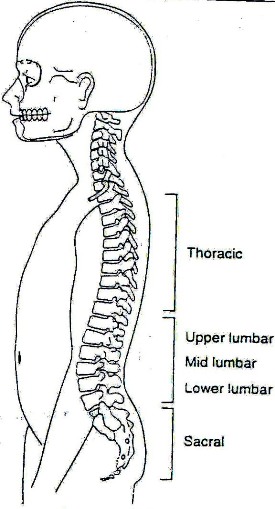
In spina bifida, the nerves are damaged because the spinal cord has not formed properly. The amount of nerve damage varies greatly and can depend on where the lump is on the back. See Fig. 19.3.
Figure 19.3: Spina bifida location
If the spina bifida is at the:
Thoracic Level:
- The child will not be able to stand up by him or herself.
- He/she will require high level bracing and splinting to stand.
- He/she will need a wheelchair for mobility.
- Common deformities are kyphosis, scoliosis, hip dislocation, knee contractures, and clubfeet.
Upper Lumbar Level:
- The child will usually not be able to stand up by him or herself.
- He/she will require braces and crutches to walk.
- He/she will probably need a wheelchair.
- Common deformities include hip dislocation, knee contractures, and clubfeet.
Mid Lumbar Level:
- The child may have some ability to walk by him or herself with aids.
- He/she will require bracing.
- He/she may not need a wheelchair.
- Common deformities are hip flexion contractures, hip dislocation, clubfeet, and calcareous feet.
Low Lumbar and Sacral Level:
- The child will usually stand at a normal age.
- Walking by him or herself may be delayed.
- Child may need braces for ankles but not use crutches to walk.
- Common deformities are club feet, foot and toe deformities.
Well, the main effects of nerve damage in spina bifida are as follows:
- Muscle weakness or paralysis. Paralysis can be of two different types:
- Spastic (muscles feel stiff): Where the spinal cord is normal below the level of spina bifida, there may be reflex muscle activity. These movements are called spasms and cannot be controlled voluntarily.
- Flaccid (muscles feel floppy): Where the spinal cord is abnormal below the level of the spina bifida, the muscles are unable to contract even by reflex action. This type of paralysis is more common in children with spina bifida.
- Lack of feeling in the skin.
- Lack of bowel and bladder control.
Assessment of an Infant with Spina Bifida
When an infant with spina bifida is born, he/she should be seen by a doctor immediately. The infant will usually require an operation to repair the spina bifida and may need to stay in hospital for some time. When the infant returns from the hospital, it will be very important to assess him/her carefully and to develop a treatment plan. This plan will assist you in developing special exercises that will help to promote his/her development. It may be done in consultation with the physiotherapist or occupational therapist.
It is important to assess when the infant is first seen. This information can also help when you are developing your plans for treatment.
Assessment of the infant with spina bifida must cover several areas. These include:
1. Presence or absence of movement in the legs:
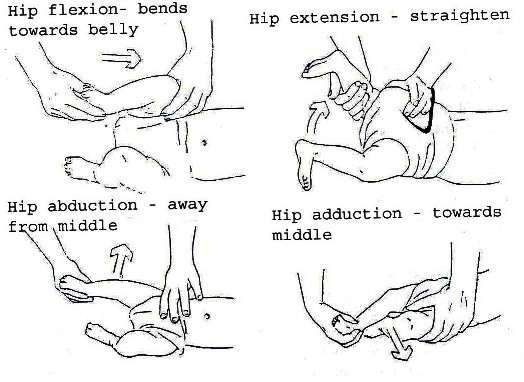
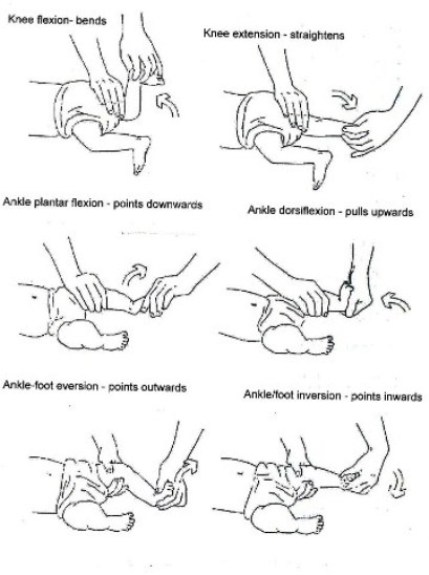
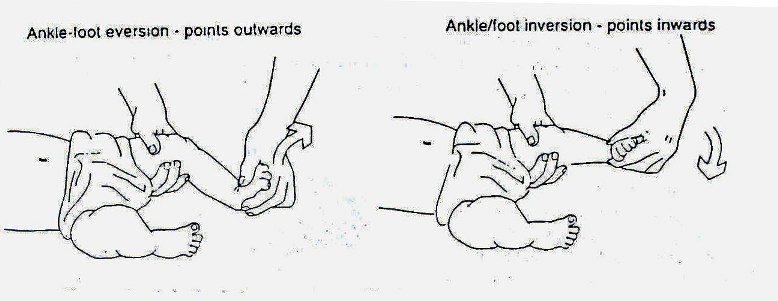
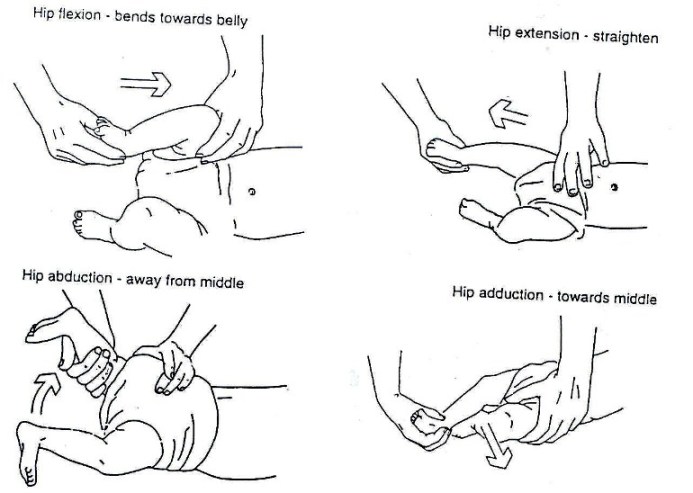
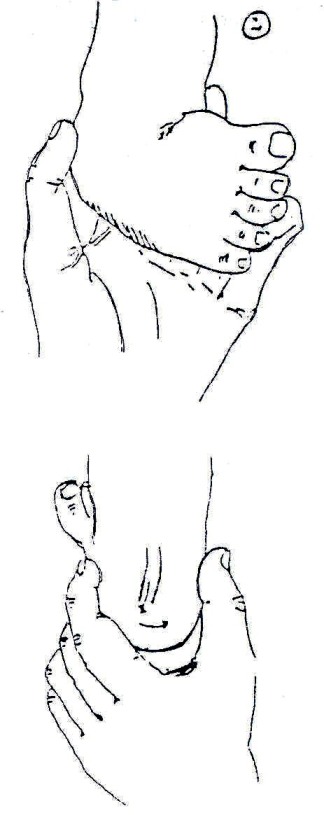
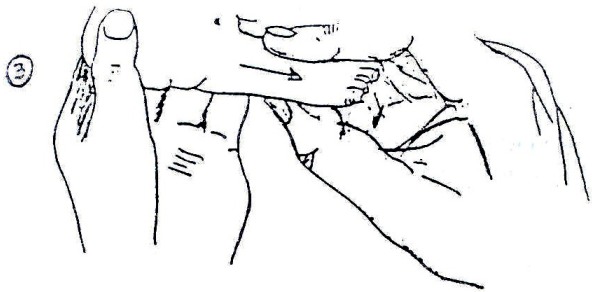
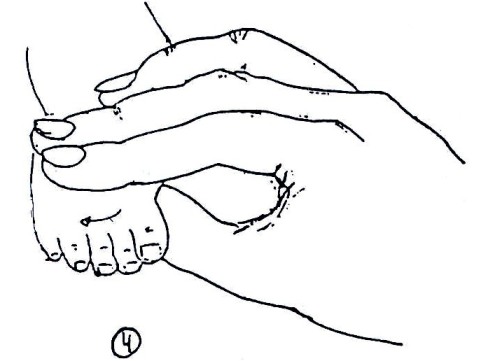
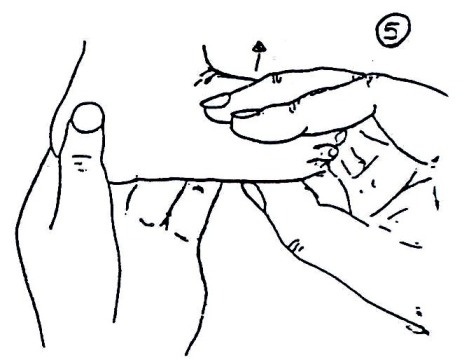
At the first assessment, movement in the infant’s legs should be looked at. The presence or absence of leg movements should be observed and recorded on an assessment form with a picture like that in Fig. 19.1.4. A muscle chart is a useful way of recording these movements. Rather than looking at each individual muscle in the leg, look at the movement at each joint to see if it is present or not. The following diagrams in Fig. 19.1.4 shows what the joint movements are called. The diagrams show the movements being guided by the hands. When you are observing active movement, do not place your hands on the infant; just watch to see what the infant can do on his/her own. See Fig. 19.1.4.
The strength of muscles should also be graded and recorded using the following muscle strength grading:
0 = no contraction
1 = contraction, no movement
2 = movement without gravity
3 = movement against gravity, no resistance
4 = movement against gravity, with resistance
5 = normal strength
Fig. 19.4: Assessing Movement in the Legs
It is difficult to record accurately the strength of an infant’s movements. This is best done when he/she is awake, as you need to see what movements he/she can do on his/her own. Talking to the infant and holding toys or brightly coloured objects in front of him/her may stimulate movement. It can also help to look at the movements in the infant’s legs when he/she is crying, as he/she may move more at this time.
It is important that the movement in each leg is recorded separately as there is often a difference in the strength of each leg.
2. Presence or absence of feeling in the legs:
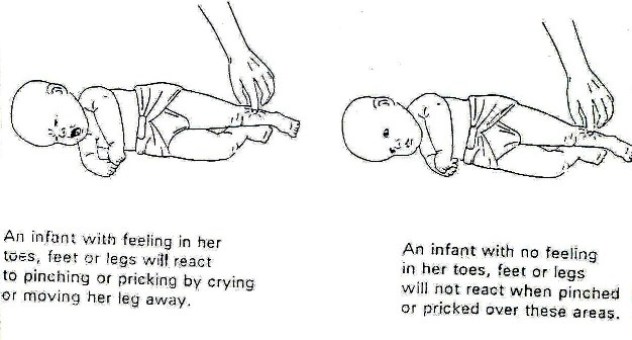
It is difficult to assess the loss of feeling in the legs of an infant with spina bifida. You may be able to see where he/she feels by looking at his/her face and breathing to see if he/she reacts to touch.
The best way to do this is to use a light pinch or prick with a pin over the toes, feet and legs. The infant’s reaction, such as pulling away, crying, or no reaction, should be recorded on an assessment form with a picture like that in Fig. 19.5. Colour in the areas on the form where you think the infant does not feel.
Figure 19.5: Assessing the infant for feeling
3. Presence of other abnormalities
4. Assess the size of the head by measuring the head circumference
Regular Assessment of the Child:
As the child grows and develops it is very important to assess him/her regularly. Movement skills, contractures, and deformities can change over time due to unequal muscle strength. The child should also be progressing through the developmental stages of movements, such as sitting, standing, and walking.
A regular reassessment (at least every three months) will indicate if the child’s treatment programme is appropriate and effective.
It is necessary to record:
- Child’s developmental progress
- Changes in movement and feeling of lower limbs
- Development of deformities or contractures
- Changes in the shape of the child’s spine
- Problems that might arise as a result of hydrocephalus
- Problems with urine and stools
- Family concerns about the child
This assessment form can be used for both the first assessment and for ongoing assessment (Fig. 19.6). Always keep a record of the child’s progress so that the treatment plan can be changed as the child changes. One way of doing this is to develop a problem list from the assessment form (see Table 19.1) and then decide upon a plan of action in consultation with the parents. A copy of this action plan should be given to the parents. This should be updated regularly and recorded as follows:
Table 19.1: Sample Record of Problems |}
| DATE | PROBLEM LIST | ACTION PLAN |
Problems Associated with Spina Bifida Occulta:
In the milder forms of spina bifida, the children usually do not have abnormality of the spinal cord or nerves and so there are no leg, bladder or bowel problems.
Spina bifida occulta can rarely be associated with abnormal development of the spinal nerves and the spinal cord. These abnormalities can cause the spinal cord to attach to the spine (tethering).
In these cases the following may be seen:
- Loss of strength, feeling and co-ordination in the movements of the legs, mostly asymmetrical.
- Abnormalities of the feet, such as clubfeet, and clawing of the toes.
- Poor development of the muscles of the lower legs.
- Altered bladder and bowel function with retention of urine and constipation.
ASSESSMENT FORM FOR CHILDREN WITH SPINA BIFIDA
NAME:_______________________________ DATE OF ASSESSMENT:________________________ DATE OF BIRTH:_______________________________ ADDRESS:_______________________________ HYDROCEPHALUS:_______________________________
MEASUREMENT OF HEAD SIZE:_______________________________
MUSCLE CHART:_______________________________
| LEFT | MOVEMENT | RIGHT |
|---|---|---|
| Hip flexion | ||
| Hip extension | ||
| Hip abduction | ||
| Hip adduction | ||
| Knee flexion | ||
| Knee extension | ||
| Ankle plantarflexion | ||
| Ankle dorsiflexion | ||
| Ankle eversion | ||
| Ankle inversion |
GRADE MUSCLE:
0 = No contraction
1 = Contraction, no movement
2 = Movement without gravity
3 = Movement against gravity, no resistance
4 = Movement against gravity, with resistance
5 = Normal strength
DEFORMITIES OR CONTRACTURES PRESENT:
1._______________________________
2._______________________________
3._______________________________
4._______________________________
5._______________________________
6._______________________________
7._______________________________
Treatment of spina bifida occulta:
The child with spina bifida occulta should be assessed regularly for changes in the strength and feeling of the legs and in bowel and bladder function.
If there is abnormal function, then the problems should be dealt with in the same way as those in severe forms of spina bifida.
If tethering of the spinal cord causes major problems, surgery may be necessary.
Assessment of contractures and deformities:
When an infant with spina bifida is born, some joints or muscles in the legs may be contracted or deformed. This happens because some muscles are stronger than others. It can also happen when joints do not move and stay in one position for long periods of time.
A contracture is a shortened muscle that prevents the full range of movement being carried out at a joint. The joint may become stiff.
Hip and leg will not lie flat on the floor. Figure 19.7: Contracture of the Hip
A deformity is an abnormal position of a joint. The joint may not move at all.
Fig. 19.8
Fig. 19.9
At the first assessment of an infant with spina bifida, all limbs should be checked, including the upper limbs. This is done by moving all joints in the arms and legs through a full range of movement. Any joints that are tight or contracted should be recorded on an assessment form (see Fig. 19.6)
Other Assessments:
There are some further areas that should be looked at when the infant with spina bifida is assessed. These include:
- How awake and alert the infant is.
- How the infant likes being moved around.
- How much the infant cries.
- Parent’s response to the infant.
- Family concerns about the infant.
We have completed assessment and drawn a treatment plan. Let us now discuss the rehabilitation or treatment methods.
Rehabilitation Methods:
- For prevention of further disability, the following exercises are used.
- Promoting development and movement can be achieved through assisted and training of milestones.
- Building of muscle strength can be achieved through assisted and active exercise.
- Prevention of pressure sores may be achieved by avoiding keeping the child in one position for too long.
- Passive movements to prevent contractures. See Fig. 19.11 and 19.12.
- Positioning techniques. See Fig. 19.13.
- Splinting
What Is a Pressure Sore?
A pressure sore is an area of the skin that has had too much pressure and breaksopen, causing a sore. These can occur if a child sits or lies too long in one position. Sites include buttocks, heels and head.
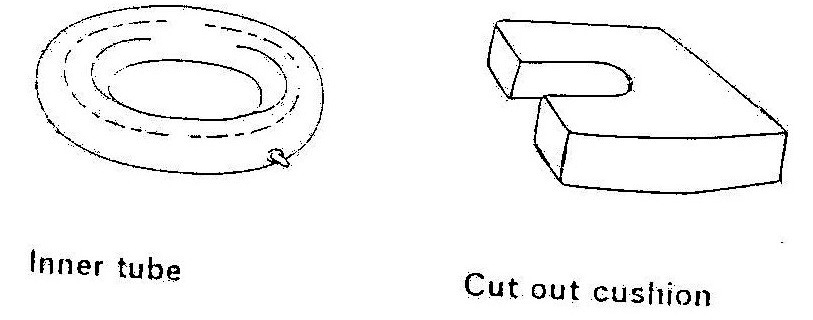
Figure 19.10: Cushions for preventing pressure sores
Figure 19.11: Passive Movements to prevent contractures.
Ankle stretches help the foot gain a good position for standing and walking. Splints and plasters can also be used to correct the position of the foot. These should be made in consultation with a physiotherapist or doctor. They should be changed regularly to prevent pressure sores or rubbing.
Hip stretches help gain the movement necessary for standing and walking. Good hip movement is also essential for other activities such as toiletting and dressing.
It is important to move each joint in the lower limbs through full range of movement every day, even if no contractures and deformities are present. This will prevent the joints from developing contractures. Each movement listed on the muscle chart should be checked (see Fig. 19.1.6)
Figure 19.12: Passive Movements to Prevent Contractures
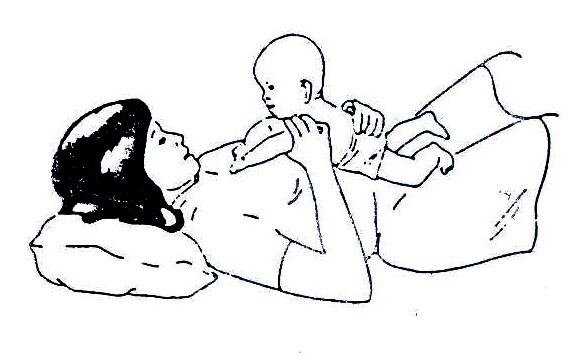
Positioning of the infant or child can assist in the correction and prevention of contractures and deformities. The child should not remain in one position for long periods of time. For the older child, make sure his/her hips are flat on the ground.
Lying on mother’s belly can make this position fun for the infant. A hand placed on the infant’s bottom can help to stretch tight hips.
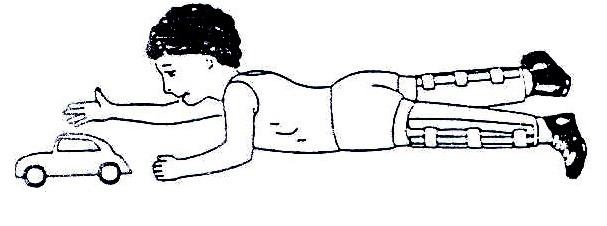
For, the older child, make sure his/her hips are flat on the ground The child or infant can be placed on his/her belly each day to prevent hips from getting tight. When the infant’s hips are tight and do not move apart easily, you can use your body to help stretch them during daily sessions
Fig. 19.13: Positioning Techniques
How are pressure sores prevented?
A child should change positions regularly. If he/she is sitting for long periods of time in a wheelchair, he/she should do pressure lifts. To do a pressure lift he/she should lift his/her buttocks off the seat by pushing up with his/her arms on the armrest or back tyres. This should be done ten times hourly. A cut out cushion may be placed on a chair under the buttocks to help prevent pressure sores.
If redness of the skin or rubbing is caused by badly fitting clothes or braces, they must be altered immediately. The child must not wear them until they have been altered.
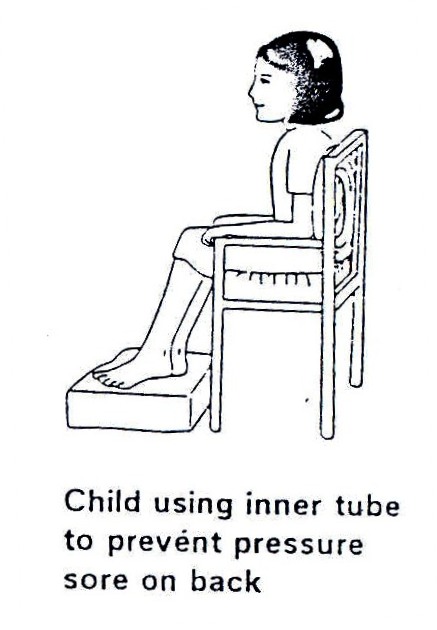
If the spina bifida on the child’s back is large and raised it may rub against the back of a chair or wheel chair. This may also cause a pressure sore. It can be prevented by placing a cushion with a hole cut out or an inner tube from a tyre, behind the child when he/she is sitting.
Fig. 19.14
What to do if a pressure sore occurs:
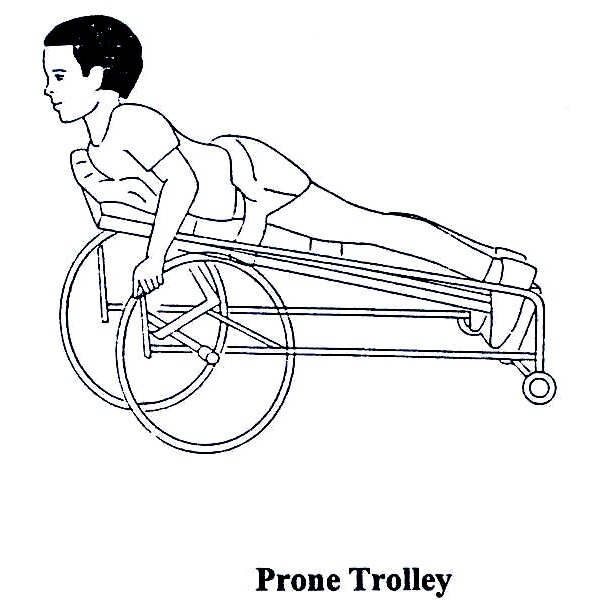
Weight must be kept off the sore until it is completely healed. The sore must be cleaned every day. If the pressure sore is too deep, it may need to be closed by surgery. The child should still be encouraged to move around if the pressure sores are on his/her buttocks. A prone trolley can be used. Lambs wool, gloves filled with water can also be used to prevent pressure sores.
Fig. 19.15: Prone Trolley
Now let us consider bladder and bowel problems.
Management of bladder and bowel:
Most children with spina bifida will have some problem with bowel and bladder control. This will vary from nearly full control to total incontinence of bladder and bowel functions. It is important that these are managed well to enable child to be healthy and to be socially acceptable amongst the members of their community.
Parents or caregivers will need to discuss the most appropriate management for their child’s bladder and bowel with the doctor or nurse from the time of birth. This will need to be regularly reviewed as the child grows and functions change.
Bladder Problems:
The child should be encouraged to drink lots of water and other fluids to help the bladder and kidneys stay well and healthy and prevent infections.
Only a small number of children who have spina bifida will be successful in gaining bladder control.
There are two types of bladders in children with spina bifida:
- Bladders that dribble with urine all the time.
- Bladders that don’t empty.
Bladders that dribble urine all the time:
This type of bladder constantly passes urine. For the infant, his/her clothes and bedding will always be wet. It is important to look after his/her skin well with frequent clothing changes and thorough washing and drying of the skin. The older child may need to wear a pad in his/her pants to absorb the urine. This must be changed regularly to prevent odour and clothes becoming wet. If the skin is left dirty, rashes, infections and open sores can occur.
Bladders that don’t empty:
The most common way of managing bladders that don’t empty is by intermittent catheterisation. This is used for two reasons:
- To keep the kidneys healthy
- To keep the child and his/her clothes dry and free of urine
Such children should be referred to specialist who can decide what to do in the circumstances available. Intermittent catheterisation may be needed but it has to be done in a sterile way to prevent urine infections.
Bowel Problems:
Most bowel problems in children with spina bifida can be managed by diet to regulate stool consistency and by toilet training.
Diet:
Food controls the consistency of the stool in all children. For children with bowel incontinence, food can be used to make the stool firmer or softer, depending on the amount of fibre it contains.
The amount of fibre can be regulated to act as a laxative (high fibre) or a constipating agent (low fibre) as necessary. Fibre in tablet or drink form can be used for children who do not get enough in their normal diet. These can be gradually reduced as the fibre in the diet is increased.
Foods that are high in fibre include:
- Whole grains (maize, sorghum, millet) and wholemeal breads
- Vegetables such as cabbage, cauliflower, spinach carrots cucumbers and tomatoes
- Legumes and nuts such as, beans, peas, groundnuts
- Fruits such as mangoes, pawpaws, ripe bananas
- Brown rice
- Most staple foods
Toilet Timing:
Toilet timing is when the child sits on the toilet at the time he/she is most likely to pass a stool. Common times for this to happen are within an hour of having a meal or soon after waking up.
It is helpful if the child can pass his/her stools out of school hours and at a time most convenient for family routines. Once toilet timing routine has been established, it should remain more or less the same for a long time.
The child should sit on the toilet for at least 2 – 3 minutes. He/she should be encouraged to bear down in an attempt to pass stool. Blowing, coughing, or laughing may help the correct muscles to work. A child should be rewarded with hugs, smiles or claps for trying, not necessarily only for producing, a stool.
Loose stools:
Frequent loose stools can often be caused by intolerance to certain foods in the diet. The most common causes are pure fruit juices and spicy foods. These should be reduced in the diet for at least three weeks. If the stool becomes firm, then the cause has been found.
Some children may pass loose stools even when constipated. This constipation should be managed by increasing fibre in the diet.
NOTE: If the child continues to have bowel problems despite management by diet and toilet timing, the doctor or nurse should be consulted.
- Answer any questions the family has about the activity
- Leave some illustrations or written instructions
From the above discussion, I believe that you are now able to effectively contribute towards a better life for a child with spina bifida. Let us now consider hydrocephalus.
19.3.1 Hydrocephalus
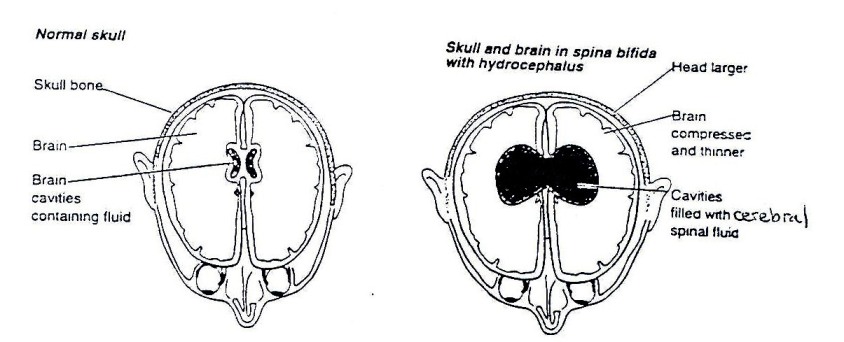
Hydrocephalus means, “too much water in the brain.” In normal circumstances, a watery fluid (cerebral spinal fluid) is produced inside of each of the cavities in the brain. This fluid flows through narrow pathways from one cavity to the next, then over the outside of the brain and down the spinal cord. This fluid is absorbed into the blood stream. Hydrocephalus occurs when the production of the fluid is greater than the absorption or when the drainage pathways become blocked. If the pathways become blocked, the fluid accumulates in the cavities, causing them to swell and the brain can be pressed against the skull. In babies, the head will get bigger, but in older children and adults the head size cannot increase as the bones that form the skull are completely joined together. This can cause severe brain damage and blindness.
What causes hydrocephalus?
Causes include:
- Spina bifida: In addition to the defect of the spinal cord, there are abnormalities in certain parts of the brain that develop before birth. These prevent proper drainage of the fluid.
- Congenital hydrocephalus: Hydrocephalus is present at birth and often has no identifiable cause.
- Prematurity: Premature babies may develop hydrocephalus because their brain has not properly developed. The blood vessels in the brain are very weak and can be damaged leading to bleeding with blockage of CSF flow. This may be temporary or permanent.
- Brain bleeding: This can occur in premature babies, children and adults, and may cause hydrocephalus.
- Meningitis or infections of the membranes covering the brain: Infection can block the drainage pathways resulting in hydrocephalus. This may happen at any age. See Fig. 19.16.
- Tumours: Swelling of the brain and surrounding tissues can result in poor drainage of the fluid.
- Genetic: Very rarely, hydrocephalus may be hereditary and may be common in some families.
Figure 19.16: Brain with Hydrocephalus
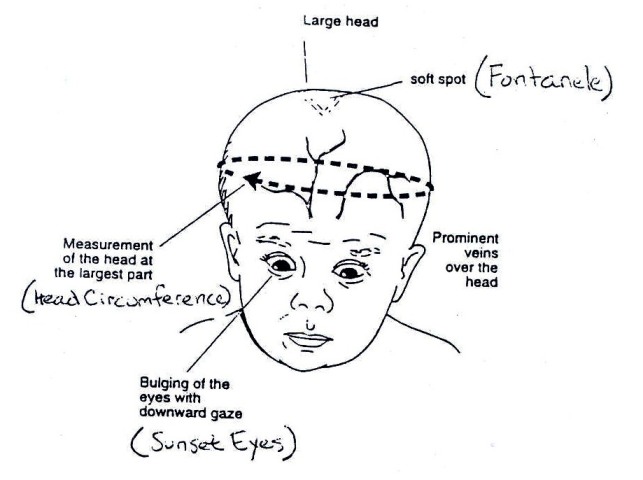
What are the signs of hydrocephalus?
The size of the baby’s head must be measured often. It should be measured around the largest part of the baby’s head just above the ears. If it starts to grow too quickly, a doctor should be seen. He/she will test to see if hydrocephalus is present.
Other signs that may be present with hydrocephalus include:
- Full or tight soft spot on baby’s head (fontanel)
- Separation of the skull bones (in infants)
- Baby appears to always look downwards (sunset eyes)
- Large veins on top of the scalp
- Irritability
- Drowsiness
- Fits
- Vomiting
Note: children with hydrocephalus have high risk of developing pressure sores at the prominences of the skull.
Figure 19.17: Signs of Hydrocephalus
How is hydrocephalus treated?
In some children, hydrocephalus requires no treatment. In others, the treatment may only be for a short time. Medicines can sometimes be used to treat hydrocephalus for short periods. Most conditions require surgical treatment by the insertion of a shunt. The shunt will not cure hydrocephalus but will drain excess fluid from the brain and prevent the condition from becoming worse.
A shunt may not be available. In this situation you will need to talk to the doctor about how to manage the child’s hydrocephalus.
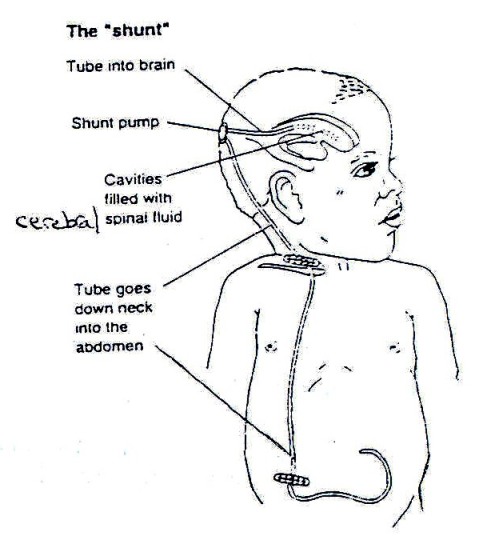
Figure 19.18: The Shunt
The “shunt” was developed to drain the extra fluid from the brain that occurs with hydrocephalus. A shunt is a small plastic tube that passes from the brain, under the skin to the abdomen. It allows the extra fluid to be drained away from the brain and absorbed in the abdomen. The shunt can be seen as it passes down the side of the neck below the ear. It then disappears deeper under the muscles into the abdomen. It is completely inside the body. When the shunt is working well, it allows the head and brain to grow normally.
Can problems occur with a shunt?
Yes, there can be problems with shunts. They may occur suddenly or developed gradually.
Shunts can become infected, blocked, or they can twist and break. The tube from the brain to the abdomen can become too short as the child grows. Surgery may be needed to remove or replace the shunt or lengthen it as needed. Medicine may be necessary if an infection is present.
It is very important for parents and health care workers to be aware of the signs of a shunt problem and to take the child to the doctor or hospital if they are concerned.
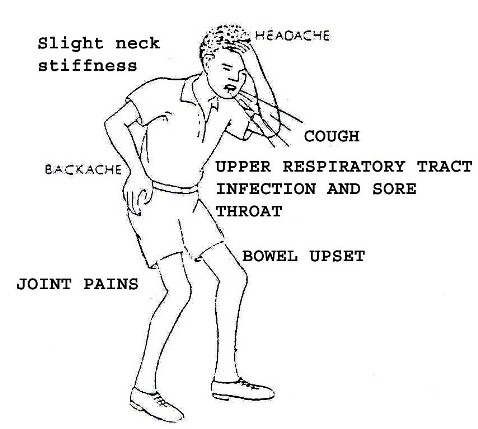
What are the warning signs of a shunt problem?
Warning signs can vary enormously between individual children and can also vary depending on the age of the child. It is important to listen carefully to the child and his caregivers about problems they may have which could be associated with the shunt. They can include one or more of the following:
- Increase in head size
- Full or tight soft spot at the top of the baby’s head until it closes at about 18 months of age
- Swelling along shunt around the pump or at the side of the child’s neck
- Vomiting
- Fever and abdominal pain
- Irritability and bad temper
- Drowsiness or sleeping more than usual
- Fits
- Visual disturbances
- Headaches in older children
When these warning signs occur, the child should be referred immediately to a doctor preferably a neural surgeon.
From the above discussions, I hope you have acquired enough knowledge on spina bifida and hydrocephalus. Let us now discuss poliomyelitis.
19.3.1 Poliomyelitis (polio)
Polio is a disease caused by a viral infection. Polioviruses are of three strains: type I, II and III. The infection is spread through faecal-oral routes in an unhygienic environment. In more hygienic surroundings, it may be spread via droplet infections through sneezing or coughing. See Fig. 19.19.
Figure 19.19: Mode of spread of polio: faecal route Note: Of the three types of polio strains, types I, II and III, infection by one strain does not protect the victim against other strains.
Presentation: In the early stages:
- A child may present with fever, running nose, cough and diarrhoea.
- There is general body aches/pains and muscle spasm..
- Severe cases will have swallowing and breathing difficulties resulting in death.
- Limbs involved may be painful to the touch.
Figure 19.20: Early Presentation of Polio
|
In early stages of polio infection the presentation may resemble malaria, common cold or diarrhoeal disease.
|
Later Stages Presentation:
The condition may progress rapidly to:
- Flaccid paralysis of muscles.
- Paralysis makes it difficult for a person to carry out activities such as walking, sitting, etc. A person’s ability to use the upper and lower limbs or various parts of the body to perform normal tasks is lost, reduced, or distorted.
- In severe cases, all limbs and trunk muscles are affected, but more often muscle groups in one or two limbs may be involved. (See Fig. 19.21)
- The paralysis of muscles is aggravated by minor trauma.
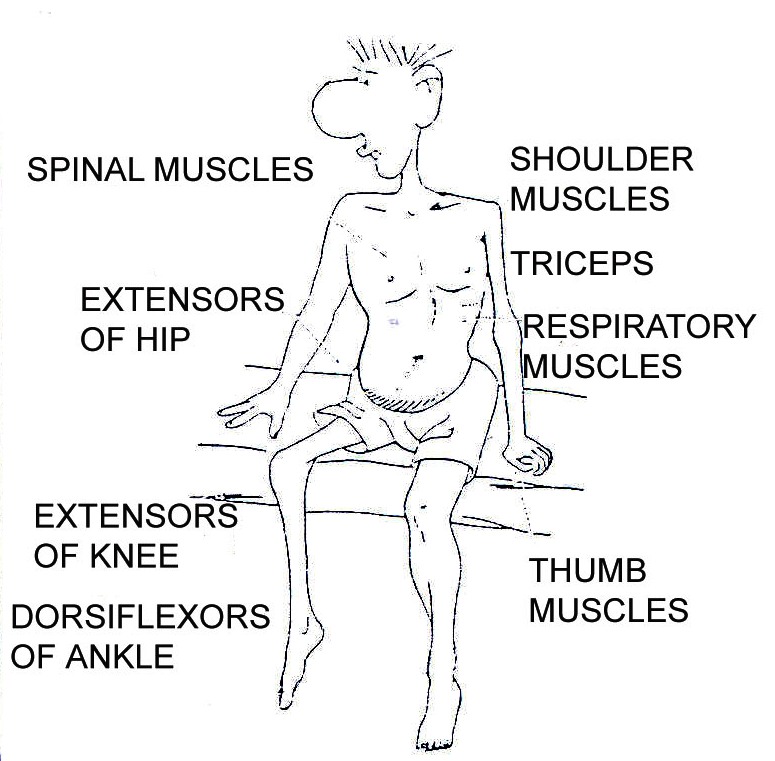
Figure 19.21: Muscles commonly affected by polio
|
Immediate Course of Action:
For the method of carrying out a clinical assessment, refer to Unit One of this Child Health Course. Some of the actions you could take at the health centre level include:
- Identify and isolate cases
- Give analgesics by oral route; paracetamol for children below 12 years, aspirin for older patients
- Carry out limited laboratory tests such as ESR, WBC, blood smear to rule out malaria
- Take a stool sample and send for further examination
- Inquire whether the child has been immunised against polio
- Refer appropriately
We have just finished discussing what happens and what can be done during the early or acute period of infection of a child with poliomyelitis. Let us now look at what happens at a later stage. We will divide this into two periods: recovery and chronic periods.
Recovery Period:
In this period the poliovirus has been killed and the undamaged areas of the spinal cord will recover. If some motor nerves were compressed (from swelling) and were not damaged, they may recover and the muscles will have normal function. If only some of the motor nerves to a muscle are destroyed, the muscle can work but it may be weak.
If all of the motor nerves to a muscle are destroyed, the muscle will be paralysed (unable to move, flaccid).
Chronic Period:
Recovery of the motor nerves is complete. No further recovery should be expected. The patient will have unchanging muscle weakness or paralysis. You will see muscle atrophy in nerve damaged muscles. After many years, bone deformities may appear from disuse, muscle imbalances, and abnormal body positions, if there is no intervention through rehabilitation exercise.
Secondary Problems Caused by Polio:
We have just discussed in the preceding section that polio causes damage to motor nerves and the nerve damage causes weakness or paralysis in different muscles of the body. Because of weakness or paralysis, a patient may begin to develop other problems, including:
- Changes in the muscle (size and shape)
- Joint deformity
- Bone deformity
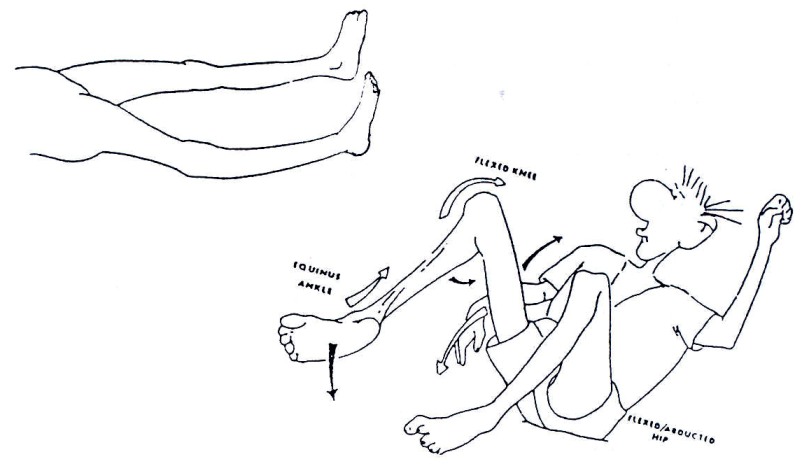
Muscle atrophy leads to a polio patient having an arm or leg that looks thinner than it normally should. If a patient puts weight on a joint that has all or part of the muscles paralysed, the joint may bend abnormally. See Fig. 19.22.
Figure 19.22: Muscle atrophy leads to a polio patient having an arm or leg that looks thinner than it normally should. If a patient puts weight on a joint that has all or part of the muscles paralysed, the joint may bend abnormally.
This can be prevented by the use of appropriate appliances. See Fig. 19.23.
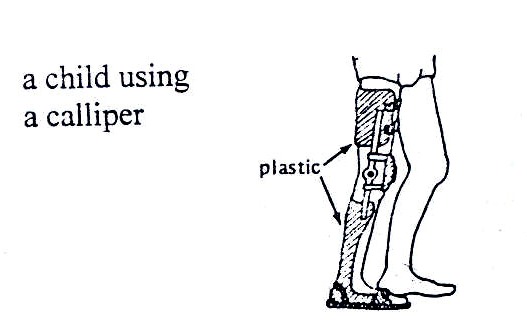
A joint bending abnormally can be prevented by the use of appropriate appliances
Figure 19.23: A child using calliper
Why do secondary deformities develop?
When the muscle does not work the fibres become completely atrophic or wasted. This changes the shape of the limbs or the affected body. Muscle wasting cannot be prevented. If one muscle is paralysed and the opposite ones are not, the length of the muscle may be modified (retracted), and the joint may become deformed (contracture). Mobilisation and right positioning of the affected joint can prevent this.
| 2
List the steps you would take to prevent children with polio in your community from getting further complications through secondary disability: _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Let us end our discussion on physical disabilities by looking at the clubfoot.
19.3.2 Club Foot
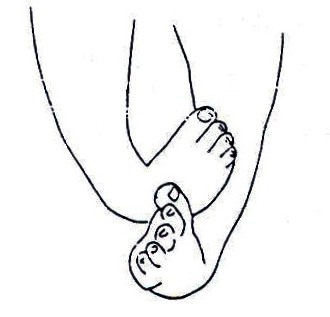
What is a clubfoot? A clubfoot is a congenital deformity of one or both feet. Congenital means that it happens before birth. See Fig. 19.24.
Causes:
The causes of clubfoot are generally unknown but from available literature clubfoot may be due to:
- The way the baby is positioned inside the mother’s womb
- Hereditary
- Associated with spina bifida
Fig. 19.24
Recognising a baby/child with club foot/feet: The identification of a child with clubfoot can be done soon after birth by observing the abnormal shape of the foot. See Fig. 19.1.25. At this stage the bones are very small and movable. As the child becomes older, the bones become bigger, harder, and very difficult to move.
In the beginning, the deformity could be only in the bone structure, but with time even the muscles can be affected. They can retract or be stretched. To prevent this complication, early treatment is important.
Fig. 19.25: Types of clubfoot
Note: If a child starts to walk on a clubfoot, the correction becomes more and more difficult.
Types of Clubfoot:
There are three types of clubfoot according to the severity of the deformity.
- Easy to correct – the foot can be put in the correct position through manipulation.
- Possible to correct but with difficulty – may fail to be completely normal.
- Not correctable by manipulation but may be possible by surgery through reconstruction.
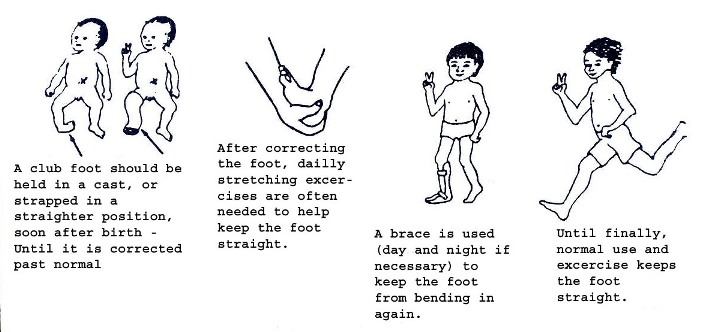
A clubfoot should be held in a case, or strapped in a straightened position, soon after birth until it is corrected. After correcting the foot, daily stretching exercises are often needed to help keep the foot straight.
A brace is used (day and night if necessary) to keep the foot from bending in again until finally normal use and exercise keeps the foot straight.
You need to check the skin carefully after removing the splint for signs of pressure sores or wounds. The foot must be mobilised when the splint is removed at least twice per day.
If the clubfoot is fixed, the child needs to be referred for surgery. After surgery, the child needs to be treated by exercises and application of splints.
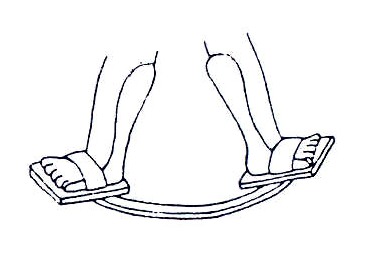
For babies under one year, or small children at night, feet can be held in a good position using a bar that joins the two feet. For a simple design, see Fig. 19.26.
Fig. 19.26: A Simple Design for a Night Brace
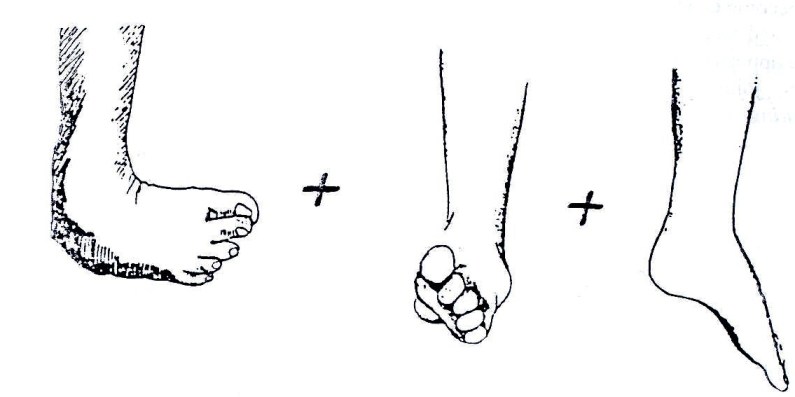
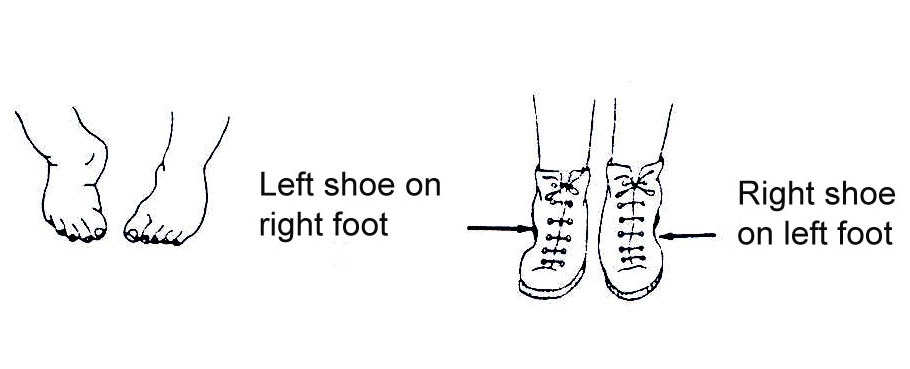
Wearing shoes in reverse – left shoe on right foot, right shoe on left foot – may also help to keep the feet corrected.
For some feet, a plastic ankle brace may work well. For more difficult feet, a metal brace may be needed, with an ankle strap that pulls the ankle inward. A light build-up on the outer edge of the shoe or sandal may also help.
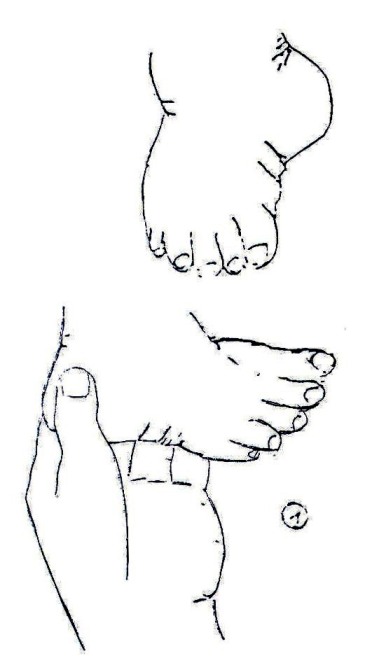
Interventions: The deformity in simple forms can be corrected by:
- Passive movements. (Fig. 19.28).
- By splinting – using simple strappings that are removable daily to allow passive movements to be carried out.
- Using plaster of paris casts that can be changed once a week.
- Putting orthopaedic shoes in reverse. (Fig. 19.27)
- Refer difficult cases to hospital as well as an occupational therapist
Fig. 19.27: For the child whose feet bend mostly at the middle or front, wearing shoes in reverse may help keep the feet corrected.
Exercises can be carried out through a series of passive movements like these.
Fig.19.28: Passive Movements and positioning
Splints or plaster casts can be used to keep the foot in the correct position.
Fig. 19.28: (Continued) Passive Movements and positioning
After correcting the foot, it is necessary to continue:
- Carrying out the passive movements
- Splinting or braces – see Fig. 19.29
- Using orthopaedic shoes in reverse – see Fig. 19.27
- Giving exercises to strengthen muscles in older children. This corrects the imbalance that, if present, would keep pulling the foot to the inside even after correction, and this would make the deformity reoccur.
Fig. 19.29: Braces for Use after Correcting Clubfeet
For all the above treatment or rehabilitation methods, one has to work with the family in order to have a positive outcome. We shall therefore discuss how to effectively work with the family.
Working Effectively with the Child and His/her Family:
Many families find it difficult to understand and remember all the information given to them at the time of the child’s birth or diagnosis of any physical disability. The future can seem uncertain for both the child and family with many difficulties to overcome. Many will be looking for a cure. A good explanation of the disability will enable the child and family to understand the condition and be able to deal with it in the best way possible.
For these reasons, it is important that you discuss the situation with the parents when their child is discharged from hospital and any other time the child is in contact with a health care provider. A successful relationship between the family and the health worker can develop the confidence to help the child to achieve the best he/she can.
It is important to always talk with the child and the family. You must explain what you are doing and why, so that they will understand. Co-operation between you, the child, and the family will help the child develop to the best of his/her ability. Be observant and patient in order to understand the child and his/her needs.
The family will need to be encouraged to treat the child with a disability like all other children in the family and not overprotect him/her. He/she should be played with, encouraged and taught as much as any other child. Praise the child and parents for each milestone achieved.
Work with the child’s family to find out their concerns and needs for the child. Listen to what they say.
You should show family members treatment activities so they can all be involved with his/her treatment programme. Do not give the family more to do than they have time for. Use a variety of ways of doing the same activity so the child does not get bored.
Points you should remember:
- Show and explain the activity you are teaching
- Guide and encourage family members in doing it
- Repeat the activity to be sure they can do it properly
- Show how the activity can be practised in daily life
We have discussed some types of physical disabilities in detail. Let us now examine some other types of disabilities, beginning with seeing difficulties.
Hearing Difficulties and/or Deafness
Hearing loss or impairment is one of the silent disabilities in our community. It is referred to as silent because it is not easy to identify a person with a hearing problem at a glance. It leads to deaf persons being referred to as fools or stupid because of a failure to respond effectively or not at all when addressed.
Causes: In children, chronic otitis media is one of the major causes of deafness and hearing problems. Other causes include:
- After-effects of meningitis
- Cerebral malaria
- Toxic doses of streptomycin and gentamycin
- Some babies are born deaf
For more information, consult Unit 11, section on ENT.
19.4: VULNERABLE GROUPS
| 3
What categories of children are more vulnerable to disability? To answer this question, make a list of children whom you consider to be more vulnerable to disability in your community: _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
I hope your list includes some of the following:
- Children who are not immunised for immunisable diseases (See Unit 4)
- Children who are born prematurely
- Children whose mothers do not attend antenatal clinics and who are delivered by untrained persons, in unhygienic conditions
- Those whose parents have defective genes
- Children who do not have proper nutrition
- Children who get fever and are not treated properly
Those are some of the vulnerable groups of children. If you recall some of the causes of disability that we discussed earlier you should realise that every one of us is potentially vulnerable to disability. Here I am referring to causes like car accidents or children falling from trees from which one can end up as a paraplegic due to injury to the spinal cord.
19.5: CLASSIFICATION
We now know the common types of disabilities that affect children in this country as well as some of the causes. Next we will look at how disabilities are classified. I am sure you are already asking yourself the question: “Why do we need to classify disability?”
It is necessary for disabilities to be classified according to severity. This guides health workers and other key players in planning services according to the needs of individual PWD or categories of PWDs
Disabilities are classified into three degrees:
- Mild disability
- Moderate disability
- Severe disability
1. Mild Disability
In mild disability the impact of the defect or abnormality is minimal on the person’s or the child’s ability to carry out activities of daily living. The child may need a simple appliance or assistive device, or a drug to overcome or control the problem.
For example, a child with a mild clubfoot may need only splinting and a specially designed orthopaedic shoe. A person with long or short sightedness only needs appropriate type of spectacles. With the help of a hearing device, a person with hearing difficulties will be able to communicate effectively. Epileptic fits are controlled with appropriate anti-convulsant drugs.
NOTE: With appropriate interventions, persons with a mild disability can lead a normal, independent life.
2. Moderate Disability
This refers to a situation where the effect or impact of the defect or abnormality requires more complicated interventions. For example, a person with bilateral paralysis of the lower limbs due to poliomyelitis needs to use callipers and crutches or a walking aid to move around.
Similarly, a child with moderate cerebral palsy may delay to develop normal milestones. However, if she or he is stimulated through specially designed exercises and functional activities, the child will develop the milestones with time. This shall be discussed later.
3. Severe Disability
Severe disability refers to a situation where the effect of the abnormality or defect is so incapacitating that the affected child cannot perform independently the activities of daily living. Such children permanently depend on family members or caretakers for their well being. They need assistance in all activities such as body hygiene, toiletry, feeding, moving, and so forth.
NOTE: Such persons are helpless and are permanently dependent on others for their survival. Now complete the following activity:
| 4
It was mentioned in section 19.5 that services for PWDs are planned according to the needs of the individual PWD. List three of the services available for children with disabilities in your community _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
19.6: SERVICES FOR PERSONS WITH DISABILITIES (PWDs)
I hope that some of the services found in your community are those listed below:
- General Medical Services: Children and other persons with disabilities who may suffer from any illness other than their disability should receive clinical treatment just like any other person. (For clinical problem solving, see Unit 1 of this course). General medical services are available in health units throughout the country.
- Specialised Medical Services: Specialised medical rehabilitation services like ophthalmology, psychiatry, orthopaedic, physiotherapy and occupational therapy services are at national and in some referral hospitals, and in some district hospitals check what is available.
- Ear, Nose, and Throat: Ear, nose and throat services are available at the national hospital. For example, Kenyatta National Hospital and few other referral hospitals. A few of these services are also offered by private clinics and at the grassroots level in areas where Non-Governmental Organisations (NGOs) operate.
Let us now discuss the following available medical services:
- Counselling
- Medical rehabilitation
1. Counselling: Disability causes stress in a family. Some couples with disabled children end up divorcing as they exchange accusations and blame each other for the disability. Family members develop negative attitudes towards the child, either due to the stigma attached to the disability or due to the abnormal posture or features that may be unsightly. The burden of special attention that the child permanently requires in severe cases makes matters worse. These children are very often neglected, isolated, and in some instances hidden in a room in the back of the house, away from the public eye. Due to cultural beliefs and ignorance, the family fears being isolated and stigmatised by their neighbours in the community.
As a health worker you can play a vital role in reducing untold suffering of children and persons with disabilities. Firstly, you have a very important role in identifying these children early. You also need to counsel the family and sensitise the community in order to create positive awareness on disability.
You can counsel the family through home visits or when the child is brought in to the clinic for other illnesses. You can also sensitise the community through seminars and discussion groups.
Apart from counselling, you can facilitate and initiate rehabilitation services or refer to the appropriate specialists. For example, in cases of physical disability you can refer the child to the physiotherapy or occupational therapy departments. Others may need to be referred to the ear, nose and throat (ENT) departments or to ophthalmology, psychiatry, or orthopaedic departments.
2. Medical Rehabilitation: Medical rehabilitation is one of the interventions that greatly improve the lives of children with disabilities. The word rehabilitation can be used to mean different things. However, in this context it is used to describe the following interventions, also referred to as medical rehabilitation.
- Provision of devices that can assist such as hearing aides (in the case of hearing impairment) and use of sign language (for communication difficulties)
- Training in the correct use of orthopaedic appliances and aides in physical disability. (See Figs. 19.1.30a, 30b, 30c and 31, and 38 through 42)
- Corrective surgery in cases of fixed deformities
- Use of specially designed exercises to build muscle strength, prevent deformities, train movement or locomotion by physiotherapy. (See Figs. 19.32 through 37
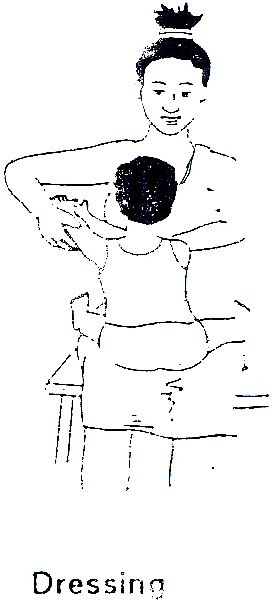
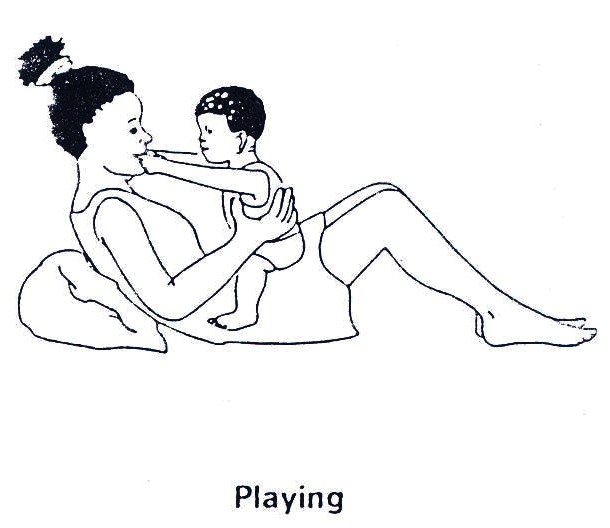
- Training in independent living by occupational therapists. (See Fig. 19.38 though 42.
19.1.7: EDUCATIONAL SERVICES
The Kenya government has a well-established special education within its Ministry of Education. It even has an institution charged with the responsibility of training teachers for special education. The master plan is to integrate children with disabilities into normal schools in order to facilitate child-to-child interaction, to avoid stigmatisation and isolation, to offer equal opportunities and ground for competition. However, there are some special education schools that were established to cater to extra special needs of some of the children.
Every district in Kenya has an Education Assessment and Resource Services (EARS) Centre. At this centre a child with disabilities can receive educational assessment and is placed appropriately.
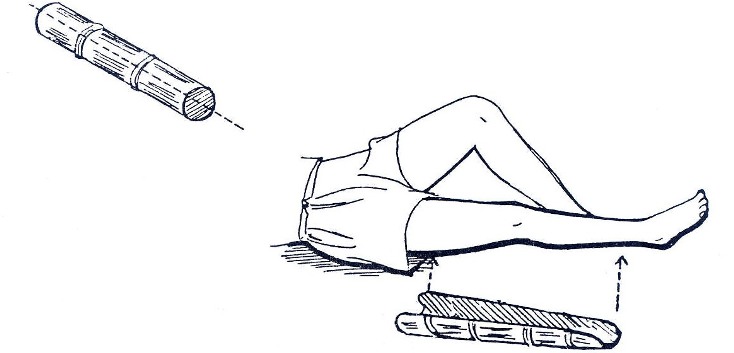
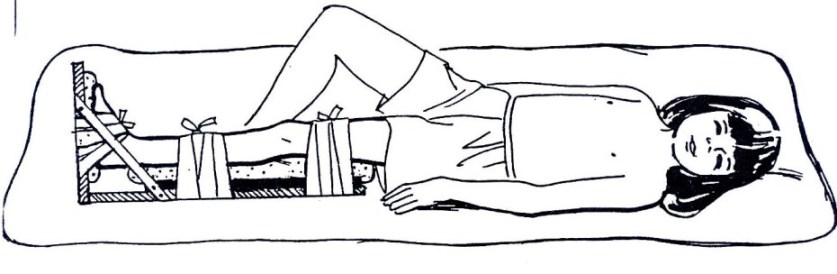
Fig. 19.30a: Bamboo Knee Splint:
You can use bamboo for knee splints, but not for the foot. If bamboo is used for a knee splint, use a sandbag to support the child’s foot in the proper position, as shown in Fig. 19.30c.
It is necessary to split the bamboo open so that the limb can rest inside the curve. Make certain that the bamboo is wide enough to fit the limb without causing too much pressure on the skin.
For a knee splint, cut one piece of the bamboo that is the length of the child’s leg from the upper third of the thigh to just above the ankle. Split the bamboo in half along its length. Trim the edges from the knee to the lower end of the splint.
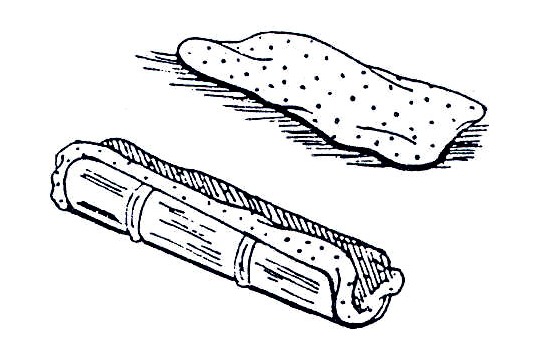
Fig. 19.30b: Put soft padding inside the bamboo to protect the child’s skin.
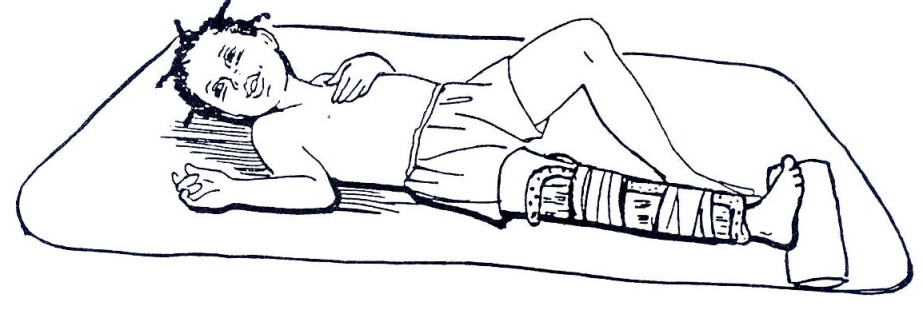
Fig. 19.1.30c: Use two strips of soft cloth to tie the splint onto the child’s leg. Use a sandbag or something firm to hold the child’s foot up.
Fig. 19.31: Foot and Knee Splint for an Older Child: Make the splint as you would make a foot splint, but make the pieces which go under the leg longer. Make the smaller piece long enough to fit under the child’s leg from just above the ankle to the middle of the thigh. Make the larger piece long enough to go under the child’s leg from the heel to the upper third of the thigh. Use three strips of soft cloth to wrap the splint to the child’s foot, lower leg, and upper leg.
Fig. 19.32: Exercises to do when the child is lying on the back:
Bend the Child’s Hip with the Knee Bent:
This exercise stretches two muscle groups. On the leg that is moved, the exercise stretches the muscles that straighten the hip. On the leg that remains straight down on the ground, this exercise stretches the muscles that bend the hip.
Begin with the child’s legs straight and close together.
Put one hand on the thigh of the leg that will remain straight on the ground.
With your other hand, gently lift the child’s other thigh up toward the trunk. Allow the knee to bend.
Then lower the thigh and straighten the leg.
Repeat the movements of lifting and bending, then lowering and straightening the leg 6 times.
Repeat the exercise with the other leg because it helps both legs.
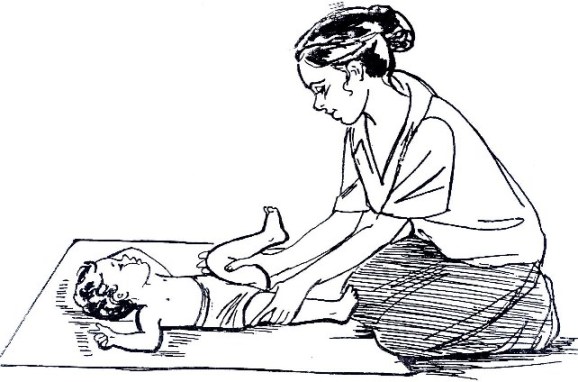
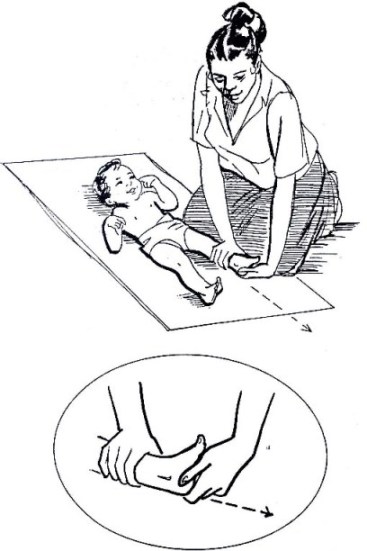
Fig. 19.33: Move the Child’s Foot Upward
This exercise stretches the muscles that pull the foot down and in.
There are two movements for this exercise. First, pull the heel (the back of the foot), then move the front of the foot upward.
Begin with the child’s legs straight.
Put one hand just above the child’s ankle to hold the leg straight down on the ground. With your other hand, grasp the heel of the child’s foot. The heel should rest between your thumb and fingers.
Gently pull the heel as if you were trying to make the leg longer. Keep pulling with your thumb and fingers, and then begin to move the palm of your hand up to the child’s foot.
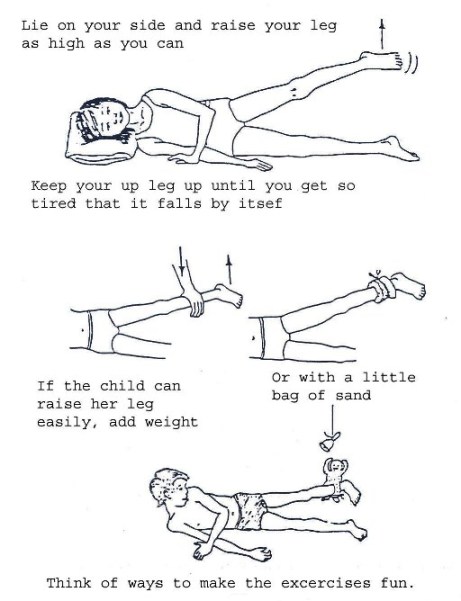
Fig. 19.34: Active Exercises
Active exercises can strengthen weak muscles. Use of appliances and assistive devices enable PWDs to perform activities of daily living despite the disability.
These rehabilitation exercises also help to make the PWD reliant and as independent as possible through learning skills in activities of daily living. For example, these exercises help a PWD to be able to move about, feed him or herself, participate in games, and so forth, and they can be used for any disability condition.
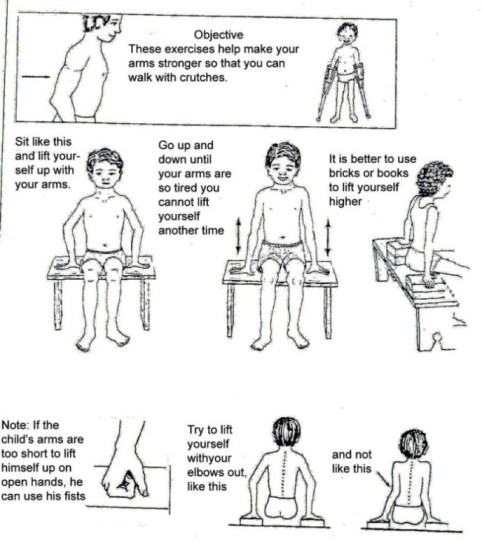
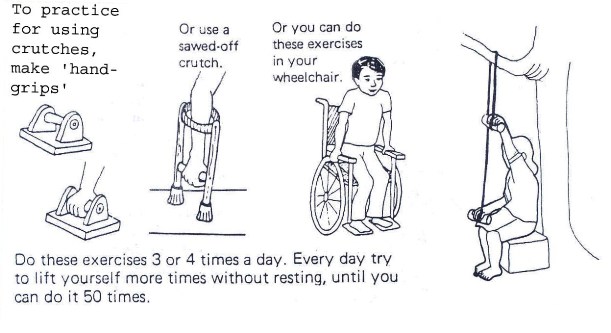
Fig. 19.35a: Exercises for Strengthening Arms – Getting Arms Ready to Use Crutches
Fig. 19.35b: Exercises for Strengthening Arms – Getting Arms Ready to Use Crutches
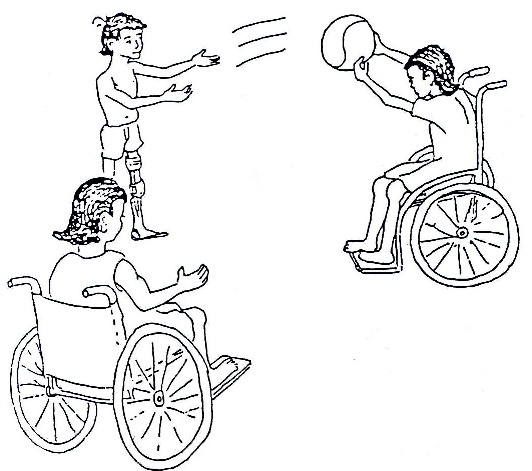
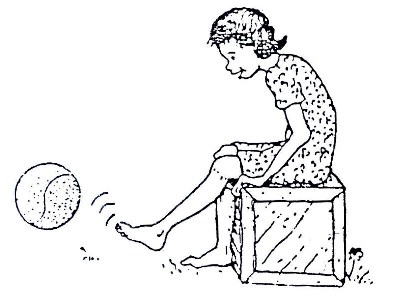
Fig. 19.36a: Sports
Fig. 19.36b: Sports
As we mentioned earlier, it is important to strengthen weak muscles AND work on improving or maintaining the general strength of the body.
Sports are a very good way to use the many muscles or the body and help to motivate the child in a positive way.
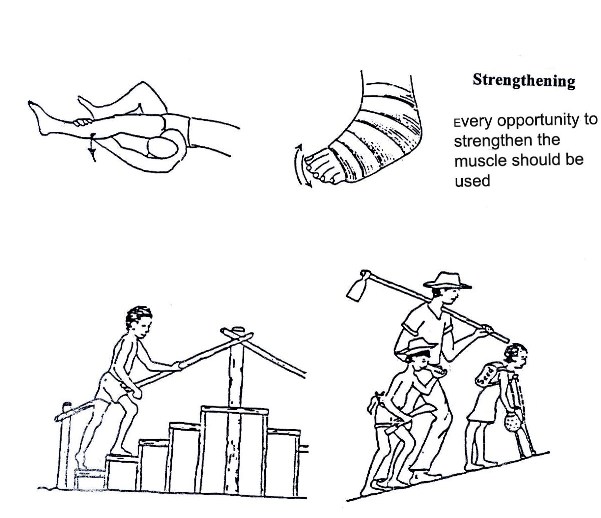
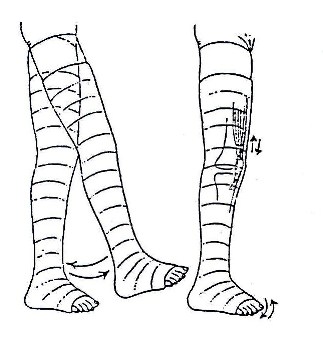
Fig. 19.37a:Strengthening
Fig. 19.37b:Utilise every opportunity to strengthen muscles
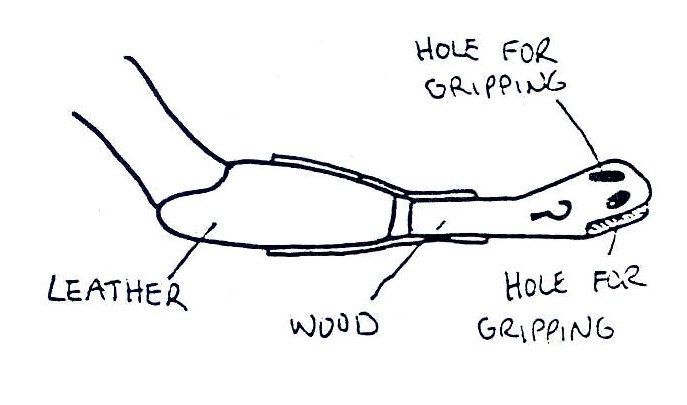
Fig. 19.38: Eating Devices for Children without Arms The picture shows a prosthetic attachment with an end part made of rubber. There are 3 holes in different directions to hold handles in different positions. Such a prosthesis can help a child without arms eat independently
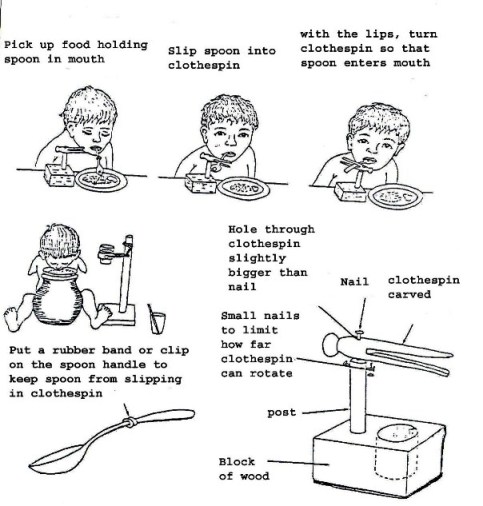
Fig. 19.39: Assistive Devices for Eating A device to assist in eating such as a clothes pin and wood can be built to enable a child without arms to eat using the mouth only.
Fig. 19.40: Methods to Make a Handle Bigger for Easier Gripping
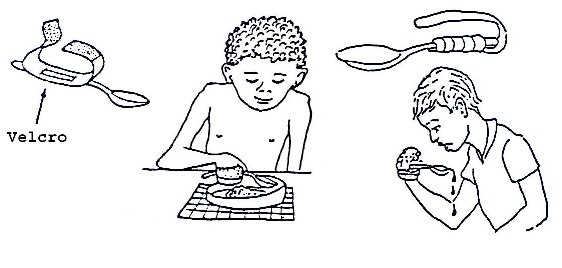
Fig. 19.41: Methods to Attach a Spoon, Fork, and Knife to a Child’s Hand
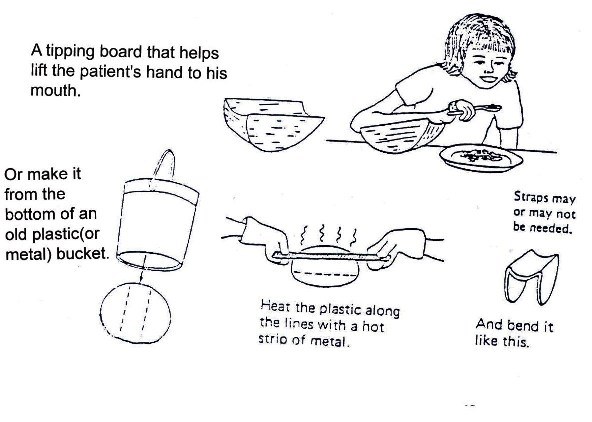
Fig. 19.42: Eating Devices for Children with Weak Arms
Note: for all these cases if in difficulty get experts such as an occupational therapist who will help and design functional aids to daily living.
19.1.8: COMMUNITY BASED REHABILITATION
We have so far discussed the various methods of providing rehabilitation services for PWDs at institutions. We have also mentioned a few of the actors in this process. However, there is one method that enables service to be provided at grassroots levels, such as within homes. This method is known as community based rehabilitation.
This motivates the community to get actively involved because they feel that they own the programme. Some modes of involvement have already been discussed in earlier sections of the text.
Complete the following activity before continuing with your reading:
| 5
We all belong to one community or to another. As a health worker, what methods would initiate community participation in your catchment area? List a few examples: _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Check your answers as you read on:
You can create awareness by organising seminars and discussion groups and workshops within the community – such as at village, sub-county and county levels.
You can also involve the community members in planning the activities. This can be more effective and beneficial if it is done in conjunction with:
- Local leaders
- Extension workers of relevant cadres in the catchment area
- Any other collaborators
During these workshops, seminars and group discussions, the following topics should be covered:
- Disability as a problem in the community
- Prevention of disability
- Cultural beliefs, superstition, and stigma associated with disability
- Types of disability and causes
- Simple techniques of management
- Available services, medical, educational facilities and socio-economic empowerment
- Way of accessing and providing these services and referral channels within the health system and outside
In this section we have stressed the fact that in order to provide integrated and holistic services to disabled children, one needs to work with actors from the community, extension workers, and other sectors. You also need to work with health workers who specialise in various fields.
| 6
Who are these actors in various fields within your community with whom you must work to provide the best services to disabled children? List them here _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
I hope your list includes the following categories:
- Health workers specialised in various fields, for example, ophthalmologists (eye specialists), physiotherapists, occupational therapists, psychiatrists or mental health workers, ENT (ear, nose, throat) specialists, clinical ophthalmic officers, orthopaedic surgeons, and so forth.
- Special education teachers
- Social workers and counsellors
- Physical planners for access to buildings
Assessing the whole child
When you get a child with a disability it is important to assess the whole child. Nutrition of the child is important. Many disabled children are malnourished. Both over and under nutrition can easily occur. Ensure that nutritional counselling is done according to the nutritional status of the child (unit 5 in these series). Some children have multiple disabilities. Make sure that all are assessed adequately. With this in mind, coordination between clinics is important so that the parent does not spend too many days attending different clinics.
In the previous section, much emphasis was placed on rehabilitation services provided by health professionals with expertise in these fields. These include physiotherapists, occupational therapists, ear, nose, throat specialists, psychiatrists, orthopaedic officers, and so forth. This category of health workers is normally stationed at tertiary and district levels. In the next section, we shall look at services at lower level units.
Before we begin, complete the following activity:
| 7
List a few roles that health workers at rural health units should be able to play: _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Now compare your answers with mine:
Health workers roles at rural health units and dispensaries include:
- Offering clinical treatment of all sick children they see and refer appropriately (for more information on clinical management, see Unit 1 of this Child Health Course)
- To identify children with disabilities in their catchment areas
- Initiate and facilitate rehabilitation activities and make appropriate referrals
- Counsel families as necessary
Parents and family members play a central role in the process of rehabilitation of children with disabilities. It is therefore important that the health worker counsels and trains them adequately so that they accept the child and develop a positive attitude towards him/her. This guards against abuse, rejection and isolation.
A family that has been sensitised takes an active role in rehabilitation of the child. For example, they will continue giving the child prescribed drugs or exercises that they were taught. They will also ensure proper use of appliances and assistive devices.
A positive attitude by the family helps in influencing the attitude of the community. It removes the stigma and minimises the tendency for isolation that the child and family normally suffer. It also helps to dispel the myths or superstitions and cultural beliefs associated with disability.
The Role of the Community: The community can play a big role in reducing the negative attitudes associated with disabilities through:
- Providing moral support.
- Active participation in all activities that create awareness in order to avoid stigmatism and isolation of a family of a child with disabilities.
The Role of Adult PWDs (Persons with Disabilities) in the Community: You must be wondering what role an adult PWD has to play. After all, they are living evidence of the negative aspect of disability. Well, other disabled persons in the community can assist you in the following ways:
- Campaigning for prevention of disabilities
- Advocacy for equalisation of opportunities for children through provision of appropriate health interventions and educational opportunities.
- Improving accessibility to public facilities such as school buildings and means of transport.
19.9: PREVENTION
We have discussed what disability is, the causes, and associated problems. Let us now look at the preventive measures against disability.
Considering some of the causes listed in the text, some types of disabilities can be prevented by the following measures:
- Immunising children against all immunisable diseases
- Expectant mothers should attend antenatal clinics
- They should be given health education so that they observe proper hygiene and feed on a balanced diet
- They should be delivered by a skilled health professional.
- Home environment should be hygienic, with toilet facilities. Homes should be kept generally clean with short grass and no stagnant water to reduce the number of malaria attacks and poliomyelitis
- Children should have proper nutrition
- Parents or caregivers should take any sick child to the nearest health unit as soon as possible for proper management
- Families with abnormal children or children with disabilities should take them early to the nearest health unit for proper identification, intervention, and referral
- Parents should follow prescribed regimes of drug treatment or rehabilitation exercises, use of appliances and assistive devices, and time tables for check-up clinics
With the above preventive measures, most of the disabilities can be prevented while the impact of others can be greatly reduced.
Having explained all the possible preventive measures against disability, let us now conclude our discussion by summarising the important issues raised in the text.
19.10: SUMMARY
Disability covers a wide field, but in this unit we have mainly consdered movement (physical) disability. We have covered the following:
- What disability is.
- The impact of disability on children and their families and the societies’ attitude towards PWDs and their families
- Types of disabilities commonly found in our societies
- Available facilities
- The key actors in provision of services for PWDs
- Preventive measures
PRACTICAL
Since disability and rehabilitation is in two parts, you will undertake the clinical session after unit 18. But as you study unit 18 look out for some of the disabilities outlined in this unit. You will use these for the practical assignment later.
To find out whether you have understood the major points contained in this unit, please do the Tutor Marked Assignment.
|
DIRECTORATE OF LEARNING SYSTEMS DISTANCE EDUCATION COURSES
Student Number: ________________________________ Name: _________________________________________ Address: _______________________________________ _______________________________________________
CHILD HEALTH COURSE Unit 19: Assignment Disabilities And Rehabilitation Part 1:
1. Which of these may cause paralysis in a child who has just been infected by the poliovirus? a. Lack of fluids b. Malnutrition c. Injections d. Resting in bed e. Vigorous exercise f. Treatment started too late
a. He is too late for a splint to help him b. Put his leg through passive movement exercises of all joints, five times a day c. Keep him sitting down all day so that his leg does not bend d. Children with disabilities should not go to school e. His leg will recover by itself f. Use a calliper to support the leg g. Use an artificial limb
_____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
_____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Our address is as follows:
Directorate of Learning Systems
AMREF Headquarters
P O Box 27691-00506
Nairobi, Kenya
Email: amreftraining@amrefhq.org