Lesson 11:Diarrhoea
Contents
[hide]INTRODUCTION:
Welcome to this unit on diarrhoeal diseases. As you know, diarrhoea is among the top five causes of childhood death in Kenya, therefore we need to learn very carefully how to manage it. Most deaths resulting from diarrhoea are due to dehydration, dysentery, and persistent diarrhoea. And what is important for us to learn is that diarrhoea from all causes and in all age groups can be treated safely and effectively by the simple method of oral rehydration therapy (ORT). Complete case management by use of drugs can also combat deaths from dysentery and persistent diarrhoea.
|
By the end of this unit you should be able to:
|
11.1 What is Diarrhoea?
Begin by doing this little activity.
Confirm your answers as you read the following discussion.
Diarrhoea is usually defined as the passage of three or more loose stools in a 24 hour period. Note that a loose stool is one that will take the shape of a container. In diarrhoea, stools contain more water than normal. Remember that mothers may use a variety of terms to describe diarrhoea depending, for example, upon whether the stool is loose, watery, bloody or mucoid, or if there is vomiting. It is important to be familiar with these terms when asking whether a child has diarrhoea. Infants who are exclusively breastfed normally pass several soft or semi-solid stools each day. Therefore, for them it is practical to define diarrhoea as an increase in stool frequency or liquidity that is considered abnormal by the mother.
11.2: TYPES OF DIARRHOEA
Before you read on do the following activity. It should take you 5 minutes to complete.
| 2
How many different types of diarrhoea do you know? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
There are three main types of diarrhoea:
- Acute Watery diarrhoea: This refers to diarrhoea that begins acutely and lasts less than 14 days. There is passage of frequent loose or watery stool without visible blood. Vomiting may occur and fever may be present.
- Persistent diarrhoea: We can define persistent diarrhoea as diarrhoea that begins acutely but lasts for more than 14 days.
- Dysentery: This is diarrhoea with visible blood in the stool. Important effects of dysentery include anorexia (loss of appetite), rapid weight loss, and damage of the intestinal mucosa by the invasive bacteria. The most important cause of children is shigella.
| 3
Why is diarrhoea dangerous? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Compare what you wrote with the following discussion on the main dangers of diarrhoea.
The most important are death and malnutrition. Death from acute diarrhoea is most often caused by the loss of a large amount of water and electrolytes (salts) from the body. And it is this loss that we call DEHYDRATION. Another important cause of death is dysentery.
Malnutrition is the other danger. Diarrhoea is worse in persons with malnutrition. Diarrhoea can also cause malnutrition and can make malnutrition worse because when a child has diarrhoea:
- Nutrients are lost from the body during diarrhoea;
- Nutrients are used to repair damaged tissue rather than for growth;
- A person with diarrhoea may not be hungry;
- Mothers might not feed children normally while they have diarrhoea, or even for some days after the diarrhoea is better.
To prevent malnutrition, encourage children with diarrhoea to eat small amounts of food at least six times a day.
11.3: TRANSMISSION OF DIARRHOEA
| 4
How is diarrhoea transmitted? ___________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Before we can list the infectious agents that cause diarrhoea, let us learn how it is transmitted. The infectious agents that cause diarrhoea are usually spread by the faecal-oral route, which includes the ingestion of water or food contaminated by faecal matter and direct contact with infected faeces. However, there are a number of specific behaviours that promote the transmission of these agents thus increasing the risk of diarrhoea.
These include:
Failing to breastfeed exclusively for the first 6 months of life;
- Using feeding bottles;
- Storing cooked food at room temperature;
- Using drinking water contaminated with faecal bacteria;
- Failing to wash hands after defecation, after disposing of faeces;
- Failing to wash hands before handling food;
- Failing to dispose of faeces (including infant faeces) hygienically;
- Host factors such as malnutrition, measles and immunodeficiency;
- Measles and infections, thus failing to have children immunized.
11.4 CAUSES OF DIARRHOEA
Before you read on do the following activity. It should take you 5 minutes to complete.
| 5
List down the causative organisms that cause diarrhoea. _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
We shall not go into detail on the causative organisms, however, it is important for you to know that diarrhoea in young children in Kenya and other developing countries is frequently caused by the organisms shown in Table 11.1
The most common of these are:
- Rota virus
- Enterotoxigenic Escherichia coli
- Shigella
- Camphylobacter jejuni
- Cryptosporidium
Table 11.1: Pathogens frequently identified in children with acute diarrhoea seen at treatment centres in developing countries
| Table | Pathogen | Percentage of Cases | Recommended antimicrobial based on clinical signs |
|---|---|---|---|
| Viruses | Rota Virus | 40 - 60 | None |
| Bacteria | Enterotoxigenic Escherichia coli (ETEC) | 10-20 | Co-trimoxazole |
| Shigella | Nalidixic acid | ||
| Campylobacter jejuni | 5-15 | None | |
| Vibrio cholerae | 10-15 | Erythromycin | |
| Salmonella (non-typhoid) | 0.1-1 | None | |
| Enteropathogenic Escherichia coli (EPEC) | 1-5
1-5 |
None | |
| Protozoa | Cryptosporidium | <5 | Ciprofloxacin |
| No pathogen found | <5 | None |
Note: In most case you will not have a stool culture so you will not know the causative organism. In general no antibiotic is recommended when there is no blood in the stool. The only exception to this rule is when there is a cholera epidemic. It is also important to remember that antibiotic sensitivity changes with time. So you need to keep up to date with current sensitivity pattern. In most cases of diarrhoea no antibiotic is needed. Remember what kills the child is dehydration.
11.5. ASSESSING A CHILD WITH DIARRHOEA
Now that you know what diarrhoea is, its types and its causes, let us tackle the main issue of how to assess a child with diarrhoea. You should remember that every child brought to the clinic should be carefully assessed before his or her treatment is planned. The clinical assessment you should make consists of taking a brief history and examining the child. Its objectives are:
- To detect dehydration, if present, and determine its degree of severity;
- To diagnose dysentery, if present;
- To diagnose persistent diarrhoea, if present;
- To evaluate feeding practices and determine the child's nutritional status, especially to detect severe malnutrition;
- To diagnose any concurrent illness;
- To determine the child's immunisation history, especially regarding immunisation for measles;
- To detect danger signs (signs of shock).
In unit 2 we briefly discussed the concept of Triage. Can you remember what we said? Triage is a process of rapidly screening sick children on arrival at a health facility. It helps to identify the children who require immediate emergency care. So before we go into details of assessment I want you to know how you will pick this child out from the queue.
| 6
What are the emergency signs of diarrhoea? List them down below. _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
I hope your list included the following emergency signs of diarrhoea:
- Lethargy or unconscious;
- Skin pinch goes back very slowly (in >2 seconds);
- Capillary refill >3 seconds.
Children with severe dehydration should also not wait in the queue as they can easily go into shock while waiting to be seen.
Checking for Capillary Refill
To check for capillary refill, this is what you should do. Hold the child’s hand above the trunk and press on the ball of the finger for 5 seconds. Then release and time how long the colour returns. This will be the capillary refill time. If it takes longer than 3 seconds then consider this an emergency sign. Skin pinch will be described later. When you have established that the child has no emergency sign he/she could still be severely dehydrated. So you still need to work quickly by going through the following:
History (ask):
- Frequency, duration, and type of stool;
- Take a careful feeding history and;
- Child's immunisation history.
Examine (assess):
- Presence of danger signs (signs of shock);
- Presence and degree of dehydration;
- Determine the child's nutritional status;
- Look for any concurrent illness.
Depending on your findings, your assessment should lead directly to:
- A plan for treating or preventing dehydration;
- A plan for treating dysentery if present;
- A plan for treating persistent diarrhoea, if present;
- Recommendations for feeding during and after diarrhoea;
- A plan for managing any concurrent illness;
- Recommendations regarding immunisation;
- A plan for follow-up.
We are, therefore, going to learn how the clinical assessment should be performed and interpreted in order to ensure that the above objectives are achieved.
| 7
How would you assess for dehydration. _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Assessing a Child For Dehydration
Do you remember the section on why diarrhoea is dangerous? In that section we said the main dangers of diarrhoea are death and malnutrition. Over 75% of the deaths due to diarrhoea are caused by dehydration alone. It is therefore very important to always first look for signs of dehydration, and determine its degree of severity in every child with diarrhoea. After you have assessed for dehydration, you can then assess other things such as persistent diarrhoea and dysentery. Usually both of the above steps are completed before treatment is given. However, when a child is severely dehydrated and/or has signs of shock, you should defer history taking and thorough examination so and start treatment without delay.
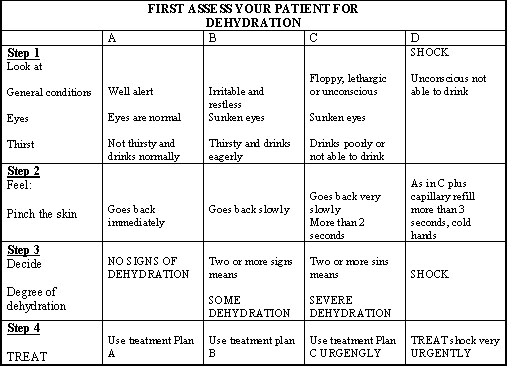
Table 11.2 can help you in assessing a child for dehydration. There are many other signs of dehydration that are not included in this table, but what we have listed are the most reliable and constant signs for a child of any age.
Ask, look, and feel for signs of dehydration: As we have already seen, the detection of dehydration is based entirely on signs observed when the child is examined. The signs that should be evaluated in every patient are as follows:
- General condition and behaviour: Observe the child carefully and see whether he appears to be:
- Well and alert
- Restless or irritable
- Lethargic or unconscious
- Signs of shock
If a child seems restless and irritable, ask the mother or the caretaker if the child is restless and irritable all the time or every time he is touched and handled. If an infant or child is calm when breastfeeding but again restless and irritable when he/she stops breastfeeding, then the child has the sign restless and irritable. Ask the mother or caretake if the child is restless and irritable at home? Many children are upset just because they are in the clinic. Usually these children can be consoled and calmed. In that case they do not have the sign restless and irritable.
- A child who is not awake or alert when they should is said to be lethargic. The child is drowsy and does not show interest in what is happening around him. Often the lethargic child does not look at the mother or watch your face when you talk. The child may stare blankly and appear not to notice what is going on around him/her.
- An unconscious child cannot be awakened. The child does not respond when touched, shaken or spoken to. Ask the mother if the child seems unusually sleepy or is difficult to wake up. Look to see if the child awakens when the mother talks or shakes the child or when you clap your hands.
- Sunken eyes: The eyes of a child who is dehydrated may look sunken. Decide if you think the eyes are sunken. Then ask the mother if she thinks her child's eyes look unusual. Her opinion helps you confirm that the child's eyes are sunken.
- Offer the child fluid: A child has the signs drinking eagerly or thirsty if it is clear that the child wants to drink. Look to see if the child reaches out for a cup or spoon when you offer water. When the water is taken away, see if the child is unhappy and wants to drink more. A child is drinking poorly if the child is weak and cannot drink without help. The child may be able to swallow only if fluid is put in the mouth.
Table 11.2 How To Assess Patients For Dehydration Weigh the child and assess as indicated
.
Pinch the skin of the abdomen:
Locate the area on the child's abdomen halfway between the umbilicus and the side of the abdomen. To do the skin pinch, use your thumb and first finger. Do not use your fingertips because this will cause pain. Firmly pick up all the layers of skin and the tissue under them. Pinch the skin for one second and then release it. When you release the skin, look to see if the skin pinch goes back:
- Very slowly (longer than 2 seconds)
- Slowly: If the skin stays up for even a brief time after you release it, decide that the skin pinch goes back slowly.
- Immediately
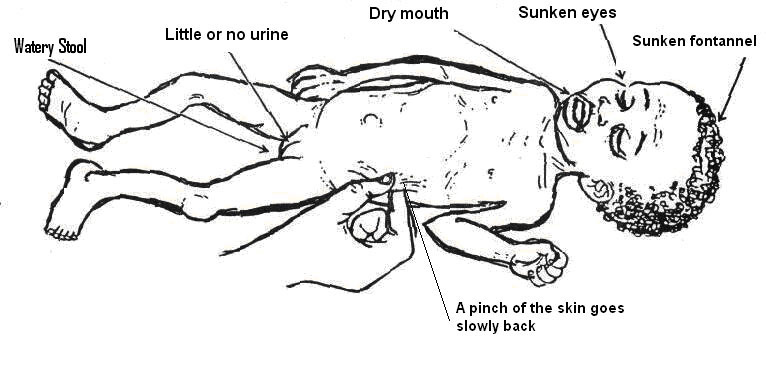
Fig. 11.1: Signs of Dehydration
An assessment and classification chart from the Ministry of Health’s IMCI guidelines is attached as Appendix 1. Study it carefully and pin it on the wall where you can easily refer to it.
Next, let us discuss how to manage diarrhoea.
11.6: MANAGEMENT OF A DEHYDRATED CHILD
Determine the degree of dehydration and select a treatment plan:
After you have done a careful assessment of the child with diarrhoea, review the findings, determine the degree of dehydration (if any) and select an appropriate treatment plan.
As we have already seen in Table11.2, the signs that indicate dehydration are organised into four columns (A, B, C and D) according to the degree of severity. If you identify two or more signs in one column, it means that the patient falls into that category of dehydration and requires the corresponding treatment plan.
Column A - No Visible Signs of Dehydration: If neither severe dehydration nor some dehydration is present, you should conclude that the patient has diarrhoea with no visible signs of dehydration.
Patients with diarrhoea but no visible signs of dehydration do have a fluid deficit which is less than 5% of their body weight. Although they lack distinct signs of dehydration, they should be given more fluids than usual to prevent signs of dehydration from developing.
Children with watery diarrhoea but no signs of dehydration should be treated at home following treatment Plan A (See Fig 11.2). This plan should be used to treat children:
- Who have been seen at a health facility for diarrhoea and found to have no visible signs of dehydration;
- Who have been treated at a health facility with Treatment Plan B or C until dehydration is corrected;
- Who have recently developed diarrhoea, but have not visited a health facility.
The four basic rules of home therapy are:
- Give more fluids than usual, to prevent dehydration;
- Give plenty of nutritious food, to prevent malnutrition;
- Take the child to a health facility if the diarrhoea does not get better;
- Give the child zinc supplement for 14 days.
Table 11.3: Treatment Plan A (Source: MOH IMCI Guidelines)
Column B - some dehydration: Look at Column B. If two or more signs are present, then the child has some dehydration. Patients with some dehydration have a fluid deficit equal to 5-10% of their body weight. These patients will need to be treated with ORS solution given by mouth following treatment Plan B (see Fig.11.4). The recommended ORS sachet in Kenya makes up half litre.
Table 11.4: Plan B: Treat Some Dehydration with ORS
Plan B: Treat Some Dehydration with ORS
These children can be treated in a special area of the clinic until the child is rehydrated. Mothers should stay with their children to help with the treatment and learn how to continue at home.
Tasks involved in Treatment Plan B: The main tasks of Treatment Plan B (Fig11.4) are:
- To estimate the amount of ORS solution to be given during the first 4 hours, for rehydration.
- To show the mother how to give ORS solution.
- To have the mother continue breastfeeding and give other fluids, as required.
- To monitor treatment and reassess the child periodically until rehydration is completed.
- To identity patients who cannot be treated satisfactorily with ORS solution by mouth and adopt a more appropriate method of treatment.
- To give instructions for continuing the treatment at home after rehydration is completed, following Treatment Plan A.
Column C - Severe dehydration: Look at Column C. If two or more signs are present, then the patient has severe dehydration. Patients with severe dehydration have a fluid deficit of more than 10% of their body weight. They are lethargic, or even unconscious, have sunken eyes and drink poorly or unable to drink. A skin pinch goes back very slowly (more than 2 seconds). Other signs include sunken anterior fontanel in infants. Some children in this category will have signs of shock which you learnt about earlier.
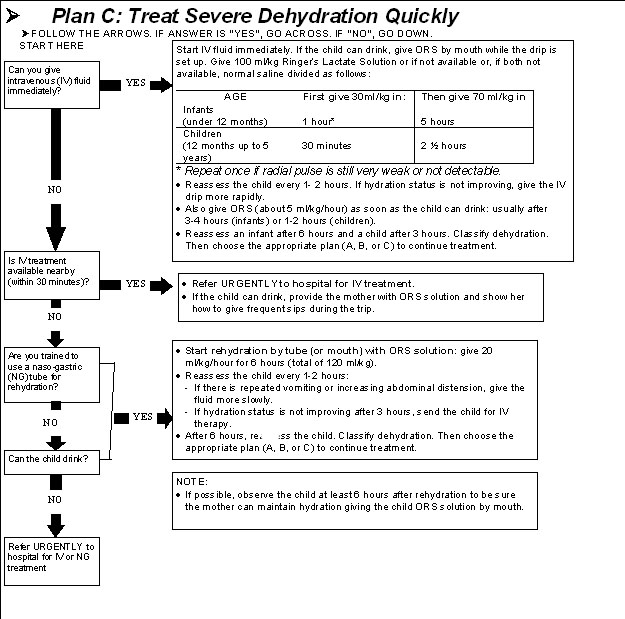
Severe dehydration requires URGENT treatment with intravenous fluids, following Treatment Plan C (See figure 11.5)
Column D – Treatment for a child in shock
Child without malnutrition:
- Infuse 20mls/kg of normal saline or Ringer’s lactate as rapidly as possible.
- Reassess and give a second dose or third if there is no improvement.
- After improvement use plan C and continue to rehydrate the child.
Child has severe malnutrition:
- Give 15mls/kg of Ringer’s lactate with 5% dextrose or half normal saline with 5% dextrose and infuse over 1hr.
Tasks involved in Treatment Plan C:
- To decide how fluid will be given: (a) by intravenous drip, (b) by nasogastric infusion, or (c) orally.
- To decide how much intravenous fluid (or ORS solution) to give.
- To give the fluid and reassess the patient frequently.
To shift to Treatment Plan B or A when the child is no longer severely dehydrated.
Table 11.5: Plan C: Treat Severe Dehydration Quickly
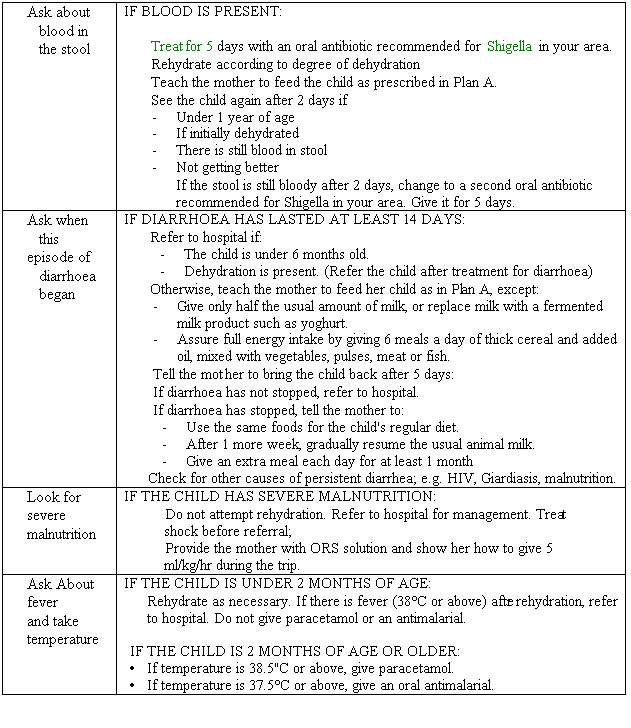
Assess the child for other problems: After assessing a child for dehydration you should remember to assess for dysentery, persistent diarrhoea, malnutrition and fever. See Table 11.6
Table 11.6: Evaluating For Other Problems
Persistent Diarrhoea:
Suspect HIV infection if you have other signs or risk factors. Children with persistent diarrhoea tend to lose more weight so ensure adequate feeding when diarrhoea stops.
Table 11.7: Give Multivatimin/Mineral Supplement for Persistent Diarrhoea
| Give Multivitamin/Mineral Supplement for Persistent Diarrhoea
Give daily for two weeks |
|---|
| Age/Weight | Multivitamin/Mineral Syrup |
| 2 months-6 months (4-8 kg) | 2.5 ml |
| 6 months-2 years (8-12 kg) | 5.0 ml |
| 2 years-5 years (12 kg-19) | 7.5 ml |
11.7: PREVENTION OF DIARRHOEA
Before you read on do the following activity. It should take you 5 minutes to complete.
| 9
What preventive measures should parents take against diarrhoea? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
Compare your answers with ours:
For any child with diarrhoea, remember to educate the family members about prevention, home treatment, adequate nutrition and the need to return if child does not get better.
You can prevent diarrhoea from attacking your child and other family members by: Giving only breast milk for the first 6 months and continuing to breastfeed for at least 2 years;
- Giving nutritious complementary foods at 6 months;
- Giving freshly prepared foods, prepared hygienically, and clean drinking water;
- Giving milk and other fluids by cup instead of feeding bottle.
- Having all family members' wash hands after passing stools and before preparing or eating food;
- Having all family members use a latrine;
- Putting a young child's stools in a latrine or burying them;
- Having the child fully immunised at the recommended age.
Epidemics:
If you see an unusual increase in the number of cases of diarrhoea, you should think of an epidemic. Using the methods of community diagnosis that you learnt in unit 6 (section 6.2) you should be able to confirm this. Remember to report and take action to stop the epidemic.
REFERRALS
We often do a disservice to our patients when we fail to refer cases we cannot manage. Seeking a second opinion is always very good. You may be able to seek a second opinion within your health facility if you have other health workers who can help. Otherwise you should refer the patient to another health facility where they can be managed.
| 10
Can you think of when you would need to refer a child with diarrhoea? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|
You should refer a child with diarrhoea if the following conditions prevail:
- If you have the knowledge but the facility where you work does not have what you need to make a diagnosis or treat the patient effectively;
- If you treat but the child keeps coming back with the same problem or takes longer than expected to respond to treatment;.
In these cases it is better to refer to the next facility or to a health worker whom you know will be able to deal with the patient’s condition.
SUMMARY
The flow chart below is a good summary of actions taken to prevent children dying from dehydration. Study, copy it and carry it with you to the practical area.
You have now come to the end of your study of Unit 9 on Diarrhoea. I hope you enjoyed learning this topic, to this unit we defined diarrhoea as the passing of three or more loose stools in a 24-hour period. We emphasised that diarrhoea is important to us as health workers because it can cause death and malnutrition. Death from diarrhoea is most often due to loss of large amounts of water and electrolytes from the body. We called this dehydration. As a health worker it is important that you recognise a child with dehydration and manage appropriately. A child with diarrhoea may have other problems that you must address so do not forget to treat the whole child rather than just the diarrhoea.
Assignment
|
DIRECTORATE OF LEARNING SYSTEMS DISTANCE EDUCATION COURSES Student Number: ________________________________ Name: _________________________________________ Address: _______________________________________ _______________________________________________ CHILD HEALTH COURSE Tutor Marked Assignment Unit 11: Diarrhoea Diseases Instructions: Answer all the questions in this assignment. Syliver is 11 months old and weighs 6 kgs. His mother breastfeeds him. His diarrhoea began 2 days ago, and he has had several very watery stools. He also vomited. His mother said there was no blood in the stools. Syliver seems alert. As the health worker examines Syliver, she finds that the skin pinch goes back slowly, and the eyes are a little sunken. Syliver drinks eagerly when offered a drink. 1. Does Syliver have signs of dehydration? If yes, describe them: _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ 2. Which treatment plan should the health worker select and follow? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ 3. How much ORS should be given to Syliver in the first four hours? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
_____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
2. Other than diarrhoea do you think Syliver has any other problem? If yes what and what will you do about it? _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________ _____________________________________________________________________
|